Seeing something unfamiliar in the toilet can instantly trigger anxiety. If you are wondering what causes jelly-like mucus in stool, it is important to first take a deep breath. A little mucus in your stool can be entirely normal because mucus acts as a natural lubricant for your intestines. Your digestive tract is lined with specialized structures called goblet cells, which constantly secrete clear mucus to help waste glide smoothly through your colon and out of your body.
However, when this natural secretion changes—becoming visible, thick, and resembling jelly—it often indicates that your gastrointestinal (GI) tract is reacting to something. Jelly-like mucus becomes a medical concern when it is new, frequent, large in amount, or paired with other symptoms like blood, ongoing diarrhea, abdominal pain, fever, or unintentional weight loss.
In this comprehensive, doctor-backed guide, we will break down exactly what causes jelly like mucus in stool, what different colors (like clear, white, or yellow) might mean, and what it indicates when it happens during pregnancy or in babies and toddlers. Let’s look at the science of your gut health, when you can manage it at home, and when it’s time to call a doctor.
Is It Normal to Have Mucus in Stool?
A small amount of mucus in the stool can be perfectly normal. As mentioned, your body needs mucin (the main glycoprotein in mucus) to protect the sensitive lining of the gut from digestive acids, bacteria, and friction. Usually, this mucus is clear and produced in such small microscopic amounts that it blends invisibly into your bowel movements.
So, when does “normal” end? Visible jelly-like mucus may happen when the intestines are actively irritated or inflamed, or when stool moves abnormally due to underlying conditions like constipation, Irritable Bowel Syndrome (IBS), a bacterial or viral infection, or other chronic bowel conditions. When the bowel lining is irritated, goblet cells go into overdrive, producing excess mucus to flush out the irritant or soothe the inflamed tissue.
Quick Summary: A small amount of mucus in stool can be normal. Visible jelly-like mucus may happen when the intestines are irritated or inflamed, or when stool moves abnormally due to constipation, IBS, or infection, or other bowel conditions.
Common Causes of Jelly-Like Mucus in Stool
Jelly-like mucus in stool can be caused by irritation or inflammation in the intestines. Common causes include IBS, constipation, diarrhea, infections, inflammatory bowel disease, and rectal inflammation. Small amounts of mucus can be normal, but mucus with blood, severe pain, fever, dehydration, or ongoing symptoms needs medical evaluation.
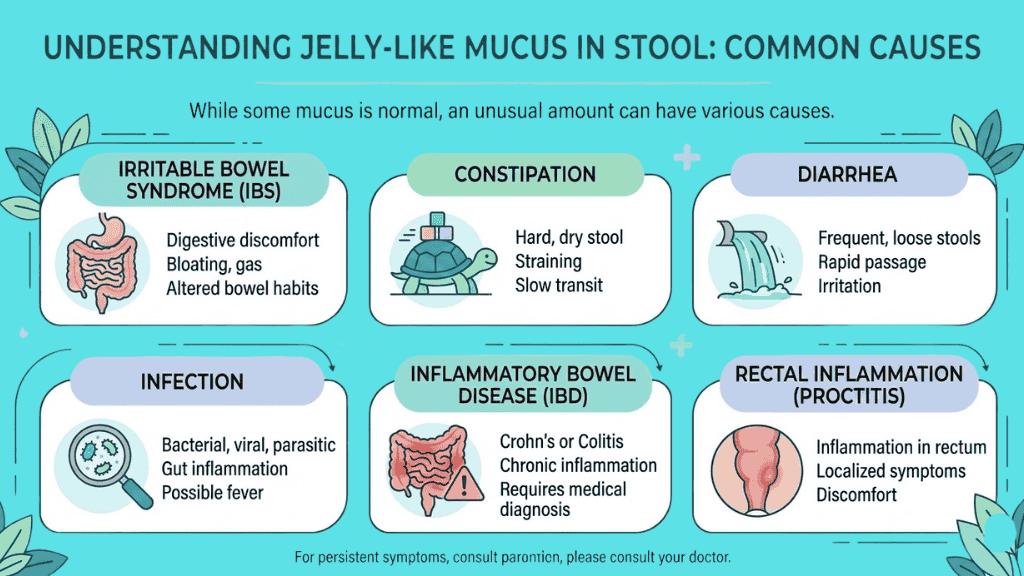
If you are consistently noticing thick, visible mucus, your GI tract is communicating that it is under stress. Below are the most common medical reasons behind this symptom.
Irritable Bowel Syndrome (IBS)
IBS is one of the most frequent culprits for a change in mucus production. It is a functional gastrointestinal disorder, meaning the gut looks normal under a microscope, but it doesn’t function normally. Medical research notes that IBS is a highly common cause of whitish mucus, which is often accompanied by bloating, abdominal pain, and fluctuating bouts of constipation or diarrhea. The exact reason IBS causes excess mucus isn’t perfectly understood, but it is believed to be linked to visceral hypersensitivity and altered gut motility.
Constipation
When stool sits in the colon for too long, it becomes hard and dry. In response to this backup, the colon’s lining may secrete extra mucus to try and lubricate the hard stool and force it out. The straining associated with severe constipation can also cause localized irritation in the rectum, further increasing mucus production.
Diarrheal Illness and Infections
Gastrointestinal infections (like food poisoning, norovirus, Salmonella, or Campylobacter) severely irritate the mucosal lining of the intestines. In an attempt to flush out the invading pathogens, the gut ramps up mucus and fluid secretion. Infections can cause sudden diarrhea with mucus, and in more severe cases, blood or a high fever.
Inflammatory Bowel Disease (IBD)
Not to be confused with IBS, Inflammatory Bowel Disease (IBD) includes conditions like Crohn’s disease and Ulcerative Colitis (UC). These are autoimmune conditions where the body’s immune system attacks the lining of the digestive tract, causing physical damage, ulcers, and intense inflammation. IBD is a major reason why someone might ask what causes jelly-like mucus in stool, as the ulcerated lining sheds mucus, pus, and often blood.
Proctitis (Rectal Inflammation)
Proctitis is inflammation specifically located in the lining of the rectum (the final section of the large intestine). It can be caused by IBD, sexually transmitted infections (STIs), or radiation therapy for cancer. Symptoms heavily feature a frequent, urgent need to have a bowel movement, passing mucus, blood, pus, and experiencing significant rectal pain.
Diverticulitis
Diverticula are small, bulging pouches that can form in the lining of your digestive system, most often in the lower part of the large intestine. When one or more of these pouches become inflamed or infected, the condition is called diverticulitis. While abdominal pain (usually on the lower left side) and fever are the hallmark symptoms, this localized bowel inflammation can increase mucus production in some cases.
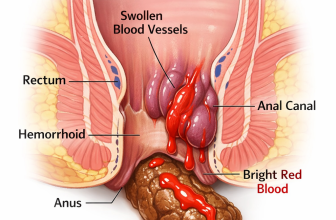
Hemorrhoids and Anal Irritation
Internal hemorrhoids are swollen veins inside the lower rectum. When they become irritated by straining or passing hard stools, they can weep a mucus-like discharge that coats the stool, sometimes accompanied by bright red blood on the toilet paper.
Rare But Serious Causes
While less common, colorectal cancer or ischemic colitis (reduced blood flow to the colon) can also present with changes in bowel habits and mucus. These belong firmly in the “red flags” category and require medical evaluation, though it is important not to jump to worst-case scenarios without a doctor’s assessment.
Diagnostic Breakdown Table
| Cause | Typical Clues | Urgency Level |
| IBS | Cramping, bloating, constipation/diarrhea, whitish mucus | Routine visit if persistent |
| Constipation | Hard stools, straining, incomplete emptying | Self-care first, see clinician if ongoing |
| Infection | Sudden diarrhea, fever, recent travel/food exposure | Urgent if severe or dehydrating |
| IBD | Long-lasting diarrhea, abdominal pain, blood/mucus, weight loss | Medical evaluation required |
| Proctitis | Rectal pain, feeling of urgency, blood/mucus | Medical evaluation required |
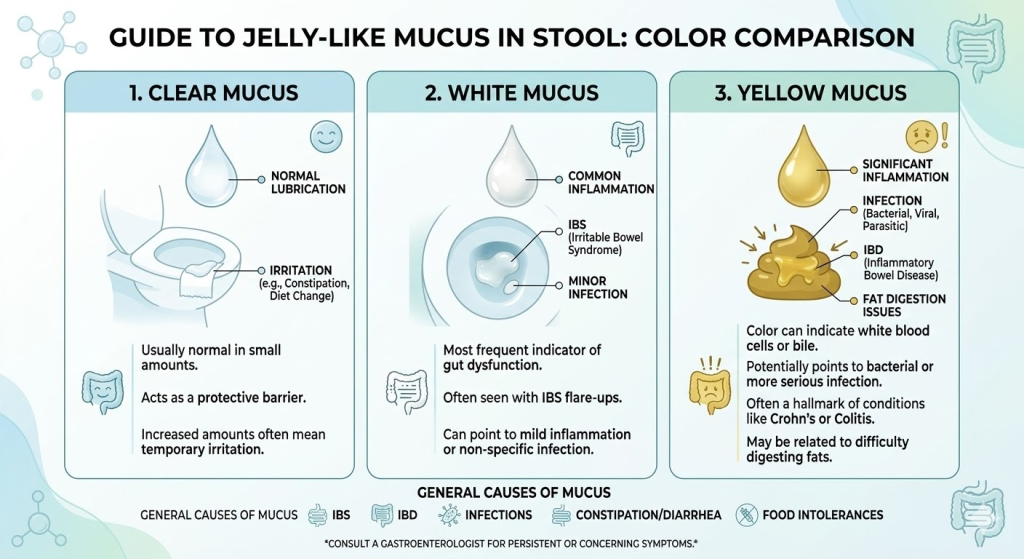
What Causes Clear Jelly-Like Mucus in Stool?
When patients ask what causes clear jelly like mucus in stool or what causes clear jelly-like mucus in stool, the answer usually points toward mild, non-destructive irritation.
Clear mucus is the most “normal” presentation of bowel mucus. It reflects the natural lubrication produced by the gut. When it becomes visible, it often means the bowel is slightly irritated but not actively bleeding or infected with a pus-producing bacteria. IBS, mild constipation, minor food intolerances, and the recovery phase after a bout of diarrhea can all fit this profile. In gastroenterology, we emphasize the pattern and associated symptoms over just the color. If the clear mucus occurs occasionally without pain or blood, it is rarely a cause for alarm.
What Causes White Jelly-Like Mucus in Stool?
If you are researching what causes white jelly like mucus in stool or what causes white jelly-like mucus in stool, you are likely dealing with functional bowel issues.
Whitish or opaque mucus is highly characteristic of Irritable Bowel Syndrome (IBS). It is specifically noted as a possible diagnostic symptom of IBS-related motility issues. It can also occur with chronic constipation, where the mucus becomes thicker and more concentrated due to the lack of water in the colon. However, if white mucus is persistent, looks like pus, or is paired with intense pain, fever, or diarrhea, it could indicate an infection or inflammation that needs a doctor’s evaluation.
What Causes Yellow Jelly-Like Mucus in Stool?
Investigating what causes yellow jelly like mucus in stool or what causes yellow jelly-like mucus in stool introduces a few different variables.
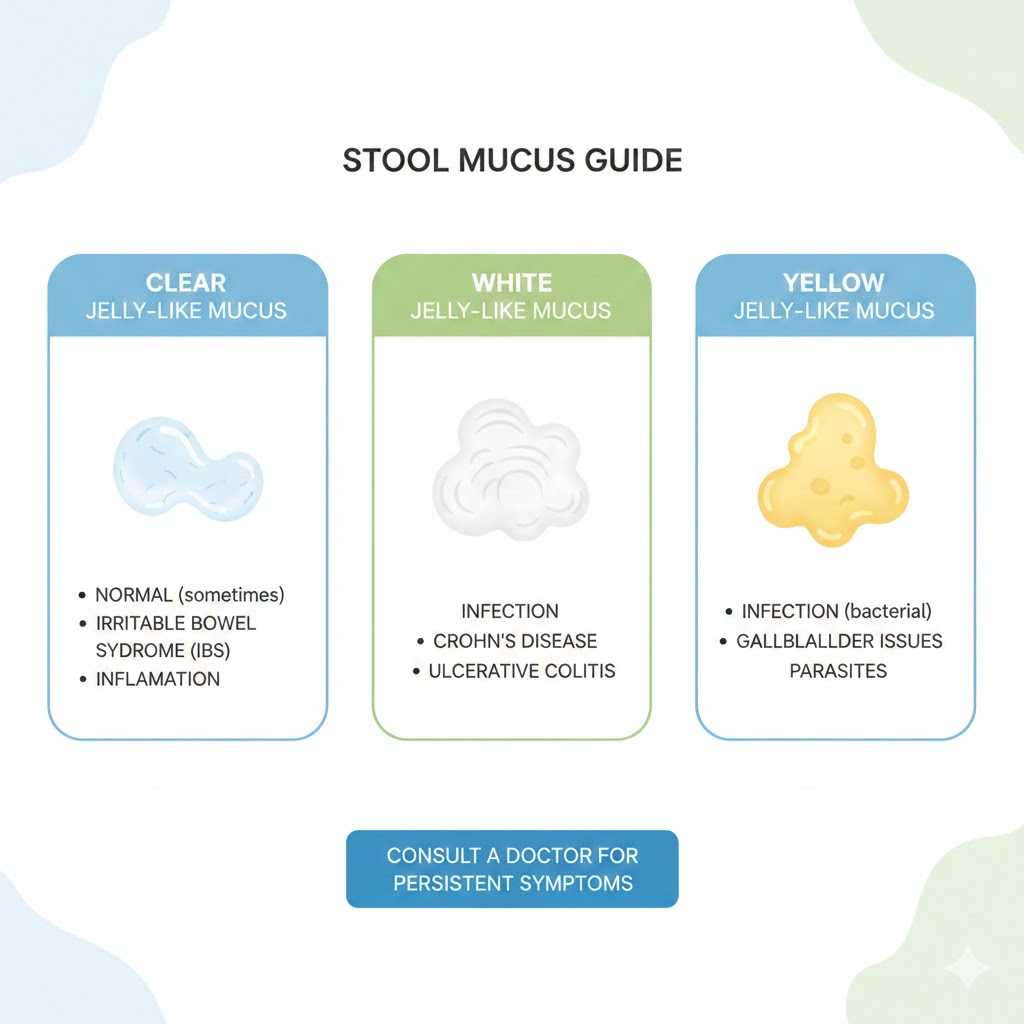
Yellow mucus can suggest a faster-than-normal stool transit time (where bile, which is yellow/green, hasn’t had time to break down). It can also point toward a mild bacterial infection, intestinal irritation, or fat malabsorption (where the body isn’t properly digesting dietary fats, leading to greasy, yellowish stools). Avoid overclaiming a single cause here. If yellow mucus is a one-off event, it may just be something you ate. However, if you pair yellow mucus with warning signs like a high fever, persistent diarrhea, or severe abdominal pain, it shifts from a simple symptom pattern to something requiring a medical diagnosis.
What Causes Jelly-Like Mucus in Stool With Blood?
This is a high-priority medical symptom. If you are asking what causes jelly like mucus in stool with blood or what causes jelly-like mucus in stool with blood, it is time to schedule a medical appointment. Blood mixed with mucus is not something to ignore or treat exclusively with home remedies.
Possible causes include infectious dysentery (a severe bacterial infection like Shigella), active Inflammatory Bowel Disease (Crohn’s or UC flare-ups), proctitis, deeper GI bleeding, severe hemorrhoids, or potentially colorectal disease.
When to Seek Help:
Jelly-like mucus in stool with blood can be caused by bowel inflammation or infection and should be evaluated promptly, especially if it happens with abdominal pain, diarrhea, fever, weakness, dizziness, or black/tarry stools.
Seek prompt emergency care if the bleeding is large in volume, if the stool looks like black coffee grounds, or if you feel lightheaded.
What Causes Jelly-Like Mucus in Stool With Diarrhea?
Figuring out what causes jelly-like mucus in stool diarrhea usually comes down to determining the difference between an acute (sudden) issue and a chronic (ongoing) one.
- Viral or Bacterial Gastroenteritis: A “stomach bug” or food poisoning violently irritates the gut lining, resulting in a rush of water and mucus into the bowels.
- Parasites: In some settings, parasitic infections like Giardia can cause prolonged, mucus-heavy diarrhea.
- IBD Flares: Ulcerative colitis frequently presents as frequent, urgent, mucus-heavy diarrhea.
- IBS-D: IBS with a diarrhea predominance can cause frequent loose stools with mucus, though usually without the fevers seen in infections.
Diarrhea from infections may include bloody stools, fever, chills, vomiting, and severe dehydration risks. Dehydration is the primary danger here, so fluid replacement is critical.
What Causes Jelly-Like Mucus in Stool During Pregnancy?
Pregnancy is a time of massive physiological shifts, leading many expectant mothers to worry about what causes jelly like mucus in stool pregnancy or what causes jelly-like mucus in stool pregnancy.
Pregnancy itself drastically changes bowel habits. Progesterone, a hormone that relaxes smooth muscle tissue to accommodate the growing baby, also relaxes the intestines, leading to slower digestion and severe constipation. This backup, as discussed earlier, triggers excess mucus. Furthermore, prenatal iron supplements are notorious for causing gut irritation, dark stools, and constipation. The pressure of the expanding uterus also increases the likelihood of developing hemorrhoids, which can secrete mucus.
In most cases, mucus during pregnancy comes from these ordinary GI causes rather than a pregnancy-specific disease. However, pregnant patients should immediately call their obstetrician or clinician if the mucus is accompanied by visible blood, persistent diarrhea (which risks dehydration for both mother and baby), severe localized pain, or a fever.
What Causes Jelly-Like Mucus in Stool in Babies?
Seeing strange diapers can be terrifying for new parents. If you are searching for what causes jelly-like mucus in stool baby or what causes jelly-like mucus in stool in babies, context is everything.

A baby’s digestive tract is still developing. Mild, clear or yellowish mucus can occur normally, especially if the baby is drooling heavily from teething (they swallow the saliva, and the mucus passes through undigested). It can also happen with minor gut irritation from a change in infant formula, the introduction of new solid foods, or a brief viral infection.
However, more urgent causes exist. Parents must be vigilant for red flags. If your baby is lethargic, has repeated forceful vomiting, a visibly swollen or hard belly, or seems in severe discomfort, call a pediatrician immediately.
A Critical Red Flag: In pediatric medicine, there is a condition called intussusception, where a part of the intestine folds into the section ahead of it (like a telescope). This causes a bowel obstruction and cuts off blood supply. A classic, late-stage symptom of this emergency is what doctors call “currant jelly stool”—stool mixed with blood and mucus that looks like dark red jelly. If you see this, it requires urgent, immediate emergency pediatric evaluation.
What Causes Jelly-Like Mucus in Stool in Toddlers?
When asking what causes jelly-like mucus in stool toddler, the landscape changes slightly as their diets mirror adults more closely.
Common causes in toddlers include chronic constipation (often due to toddler withholding behaviors or insufficient fiber/water), mild viral stomach bugs, food-related irritation (like an undiscovered dairy intolerance), or temporary bowel inflammation.
Just like with infants, you must watch for red flags: visible blood, signs of dehydration (no wet diapers for hours, crying without tears), ongoing diarrhea lasting more than a few days, unexplained weight loss, severe abdominal pain, high fever, or listlessness. If any of these occur, contact their pediatrician.
When Is Mucus in Stool a Medical Emergency?
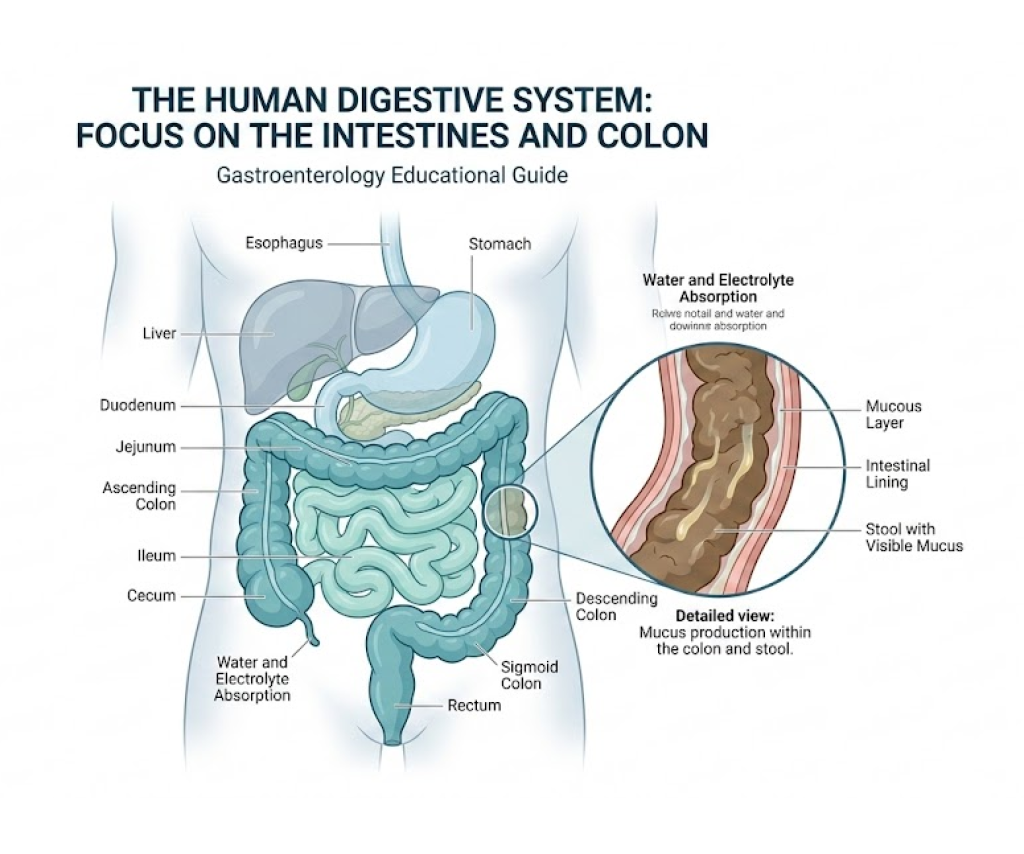
Trusting your gut—literally and figuratively—is important. While we’ve established that mucus can be normal, it is crucial to recognize when it crosses the line into a medical emergency. According to medical guidance regarding dysentery, proctitis, IBD, and GI bleeding, you should seek urgent medical care if you experience any of the following red-flag symptoms:
- Visible red blood in the stool or toilet bowl.
- Black, maroon, or tarry stools (indicating bleeding higher up in the GI tract).
- Severe, sudden, or steadily worsening abdominal pain.
- A high, persistent fever.
- Signs of severe dehydration (extreme thirst, dark urine, dizziness, confusion).
- Persistent diarrhea lasting more than 48 hours.
- Unexplained, unintentional weight loss.
- Mucus paired with forceful vomiting in infants or children.
- Intense rectal pain accompanied by blood or pus.
What is the gelatinous mucus in my poop?
That gelatinous, jelly-like substance is primarily made of mucin, a glycoprotein produced by specialized structures in your digestive tract called goblet cells. In a healthy gut, this mucus is completely normal. It acts as a protective barrier against stomach acids and harmful bacteria, and it serves as a natural lubricant to help waste glide smoothly through your colon. When your digestive system is healthy, you pass small, microscopic amounts of it every day without ever noticing. It only becomes visible and “gelatinous” when your body starts overproducing it in response to a stressor.
Why is my poop jelly like mucus?
If your stool looks like it is coated in jelly—or if you are passing mucus by itself—it means your gastrointestinal tract is irritated or experiencing a motility issue. When the bowel lining is stressed, it goes into overdrive, pumping out extra mucus to protect the tissue or flush out an irritant.
The most common reasons this happens include Irritable Bowel Syndrome (IBS), where the nerves in your gut are overly sensitive; bouts of severe constipation, where your colon secretes extra mucus to try and lubricate dry, backed-up stool; acute gastrointestinal bacterial infections; and Inflammatory Bowel Disease (IBD), which causes physical ulcers in the gut lining that shed thick mucus, pus, and sometimes blood.
Which vitamin deficiency causes mucus in the stool?
This is a great question, but it actually has the relationship backward. A vitamin deficiency doesn’t typically cause mucus in the stool. Rather, an underlying gut condition causes both the mucus and the vitamin deficiency.
When your gut lining is inflamed or damaged (from conditions like untreated Celiac disease, Crohn’s disease, or Cystic Fibrosis), it cannot properly break down food or absorb nutrients. This state of malabsorption often leads to foul-smelling fatty stools (steatorrhea) mixed with mucus. Because the gut isn’t absorbing fats correctly, you consequently become deficient in essential fat-soluble vitamins—specifically Vitamins A, D, E, and K.
What foods can trigger mucus in the stool?
Foods themselves do not turn into mucus. Instead, certain foods can irritate your unique digestive tract, prompting your gut to produce mucus in self-defense. If you have food intolerances or a sensitive gut (like IBS), the most common dietary triggers include:
- Dairy: If you are lactose intolerant, undigested dairy and lactose products ferment in your colon, drawing in water and irritating the lining, which triggers mucus and diarrhea.
- FODMAPs: These are specific high-FODMAP foods (found in garlic, onions, apples, wheat, and beans) that are notoriously difficult for people with IBS to digest.
- Gluten: For those with Celiac disease or non-celiac gluten sensitivity, gluten causes a direct inflammatory response in the intestines.
- Excessive Fats or Fried Foods: A highly fatty meal can speed up your digestive transit time or trigger bile acid malabsorption, leading to urgent, mucus-coated stools.
- Spicy Foods: Capsaicin (the compound that makes peppers hot) can physically irritate the colon lining as it passes through.
If you suspect your diet is the culprit, I highly recommend keeping a daily food and symptom diary for two weeks. Tracking exactly what you eat alongside the appearance of your stool is often the fastest way to pinpoint your unique triggers.
How Doctors Evaluate Jelly-Like Mucus in Stool
If you present to a clinic with this symptom, your doctor will play the role of a medical detective. Because gastrointestinal symptoms overlap so heavily, diagnosis requires a systematic approach.
- Symptom History: Your doctor will ask when it started, what color it is, your dietary habits, family history of bowel disease, and about any accompanying pain or bleeding.
- Stool Tests: They may request a stool sample to check for bacterial infections, parasites, or hidden (occult) blood.
- Fecal Calprotectin Test: Clinical guidelines note that a stool calprotectin test may be used when diarrhea, pain, and blood/mucus suggest intestinal inflammation. Calprotectin is a protein found in white blood cells; high levels in stool strongly suggest active inflammation (like IBD) rather than a functional issue (like IBS).
- Blood Tests: To check for anemia, systemic infection, or markers of inflammation (like CRP or ESR).
- Imaging or Endoscopy: In selected cases—especially if red flags are present or if you are over 45—a gastroenterologist may recommend a colonoscopy or sigmoidoscopy to directly visualize the lining of your colon and take tissue biopsies.
Can Diet, Stress, or Constipation Cause It?
Absolutely. The gut-brain axis is a powerful connection. Health experts emphasize that chronic stress and anxiety can directly alter gut motility and worsen bowel symptoms, particularly in those with IBS. Stress can trigger the gut to speed up (causing diarrhea and mucus) or slow down (causing constipation and mucus).
Diet plays an equally massive role. Diets low in dietary fiber and hydration lead to constipation, which, as we’ve learned, raises mucus production as the colon struggles to move hard waste. Conversely, eating highly processed foods, excessive artificial sweeteners, or foods you have a subtle intolerance to can cause mild localized inflammation, triggering a mucus response. Maintaining proper hydration and a stool consistency that is easy to pass is fundamental to gut health.
What You Can Do at Home, and What Not to Ignore
If your symptoms are mild, occasional, and unaccompanied by the red flags listed above, there are practical steps you can take at home to support your gut:
- Hydration: Drink plenty of water throughout the day. Water keeps the stool soft and reduces the need for the colon to overproduce mucus.
- Adjust Your Fiber: If you are constipated, gradually increase soluble fiber (like oats, psyllium husk, and soft fruits). If you have diarrhea, stick to bland, easily digestible foods (like the BRAT diet: bananas, rice, applesauce, toast) until it passes.
- Manage Stress: Incorporate stress-reduction techniques like deep breathing, yoga, or light walking to help calm the gut-brain axis.
- Keep a Symptom Diary: Track what you eat, your stress levels, and your bowel movements (using the Bristol Stool Chart). This is incredibly helpful data to hand to your doctor.
What Not to Ignore: Never try to self-diagnose persistent blood, severe pain, or long-lasting changes in your bowel habits. While Dr. Google is a helpful starting point, only a qualified medical professional can rule out serious conditions.
Frequently Asked Questions (FAQ)
What causes jelly-like mucus in stool?
It is typically caused by the goblet cells in your intestines overproducing mucin in response to irritation, abnormal stool transit (like constipation or diarrhea), IBS, localized infections, or inflammatory bowel conditions.
What causes clear jelly-like mucus in stool?
Clear mucus is the most normal type. When visible, it often points to mild bowel irritation, IBS, or the gut’s attempt to lubricate mildly constipated stool.
What causes white jelly-like mucus in stool?
Whitish mucus is very commonly associated with Irritable Bowel Syndrome (IBS) or chronic constipation.
What causes yellow jelly-like mucus in stool?
Yellow mucus can indicate a fast digestive transit time, a mild bacterial infection, or underlying inflammation.
What causes jelly-like mucus in stool with blood?
This is a red flag symptom that requires medical attention. It can be caused by infectious dysentery, Inflammatory Bowel Disease (Crohn’s or Ulcerative Colitis), bleeding hemorrhoids, or proctitis.
What causes jelly-like mucus in stool during pregnancy?
Hormonal changes leading to severe constipation, irritation from prenatal iron supplements, or pressure-induced hemorrhoids are the most common culprits during pregnancy.
What causes jelly-like mucus in stool in babies?
In infants, it can be caused by swallowing excess teething drool, minor formula/dietary irritations, or transient stomach bugs. However, if accompanied by blood or lethargy, it is a pediatric emergency.
What causes jelly-like mucus in stool in toddlers?
Constipation (often from withholding behaviors) and mild viral stomach bugs are the leading causes in toddlers.
Is mucus in stool always a sign of infection?
No. While bacterial and viral infections can cause it, functional disorders like IBS, dietary changes, and constipation are actually much more common causes.
Can IBS cause jelly-like mucus in stool?
Yes. IBS is one of the leading functional causes of whitish or clear mucus in the stool, often fluctuating alongside bouts of bloating, diarrhea, and constipation.
Medical Disclaimer: The information provided in this article is for educational purposes only and does not substitute for professional medical advice, diagnosis, or treatment. Gastrointestinal symptoms can overlap significantly, and an accurate diagnosis depends on your full clinical context. Always consult with a qualified healthcare provider if you experience persistent changes in bowel habits, and seek immediate emergency care for red-flag symptoms like visible blood, severe abdominal pain, or dehydration.