Discovering blood in the toilet bowl or noticing changes in your stool shape can be an incredibly alarming experience. It is a moment that often triggers immediate anxiety about serious health conditions, ranging from minor irritations to significant gastrointestinal diseases. As a physician, I understand the worry that comes with these symptoms. One of the most common questions I encounter in clinical practice is: can hemorrhoids cause bloody stools?
The short answer is yes. Hemorrhoids are a leading cause of rectal bleeding, particularly bright red blood noticed during or after a bowel movement. However, the human digestive system is complex, and not every instance of bloody stool, thin stool, or black stool is caused by hemorrhoids. While hemorrhoids are benign swollen veins in the lower rectum and anus, other conditions—some of which require urgent medical attention—can mimic these symptoms.
It is crucial to differentiate between the typical presentation of hemorrhoids and warning signs that suggest something more serious. For instance, while bright red blood is consistent with hemorrhoids, black or tarry stool is not typical and often signals bleeding higher up in the digestive tract. Similarly, persistent changes in stool caliber, such as narrow or pencil-thin stools, should not be automatically blamed on hemorrhoids without a proper medical workup.
This comprehensive guide is designed to provide clarity. We will explore exactly what kind of bleeding hemorrhoids cause, whether they can alter stool shape, and when these symptoms indicate a need for immediate medical evaluation. By understanding the nuances of these symptoms, you can make informed decisions about your health and know when it is time to see a doctor.
Can Hemorrhoids Cause Bloody Stools?
When patients ask, “can hemorrhoids cause bloody stools?”, they are looking for a direct confirmation to ease their immediate anxiety. Clinically speaking, hemorrhoids are indeed one of the most common causes of rectal bleeding.
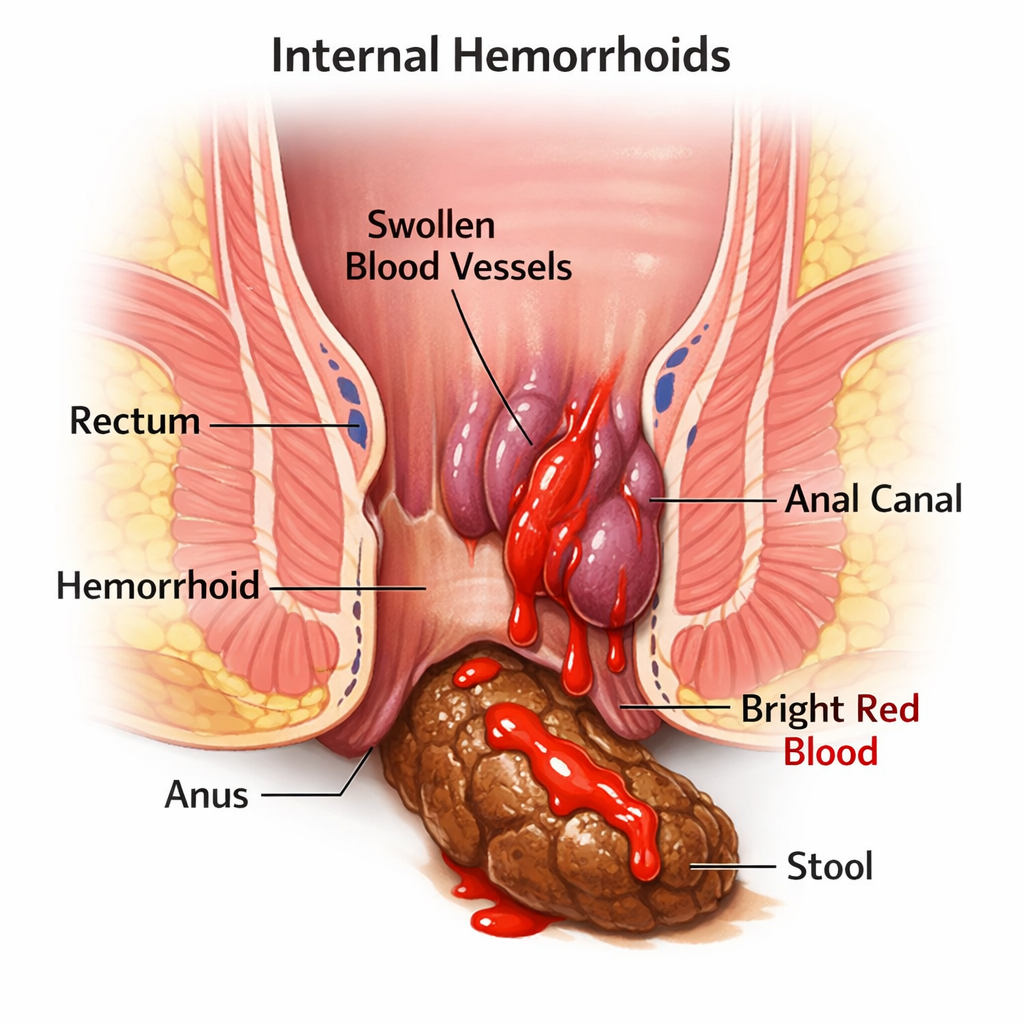
Yes, hemorrhoids can cause bloody stools. However, the characteristics of the blood are specific. The bleeding associated with hemorrhoids is typically bright red. This is because hemorrhoids are located in the lower rectum and anus, close to the exit point of the digestive tract. The blood has not been digested, so it retains its fresh, oxygenated red color.
You might notice this blood in several ways:
- On toilet paper: Wiping after a bowel movement reveals bright red streaks.
- In the toilet bowl: Drops of red blood fall into the water after the stool passes.
- Coating the stool: The blood appears on the surface of the stool rather than mixed inside it.
This type of bleeding often occurs after straining, passing hard stool, or vigorous wiping. It is important to distinguish this from other types of bleeding. If you are asking, “do hemorrhoids cause bloody stool” that is dark, maroon, or black, the answer is generally no. Hemorrhoids do not typically cause bleeding that changes the overall color of the stool to black.
Furthermore, while hemorrhoids can cause discomfort, swelling, and itching, they are not the primary cause of persistent changes in stool shape. If you are wondering, “can hemorrhoids cause bloody stool” alongside significant changes in bowel habits, such as ongoing thin stools or unexplained weight loss, these symptoms warrant a deeper investigation beyond a simple hemorrhoid diagnosis.
Yes. Hemorrhoids can cause bloody stools, but the blood is usually bright red and often appears after a bowel movement, on toilet paper, or coating the stool rather than turning it black. Persistent changes in stool shape or dark blood require medical evaluation.
What Kind of Blood Do Hemorrhoids Usually Cause?
Understanding the specific presentation of bleeding is critical for self-assessment and communicating effectively with your healthcare provider. When users search “can hemorrhoids cause blood in stool” or “can hemorrhoids cause blood in the stool”, they are often trying to gauge the severity of their condition based on the appearance of the blood.
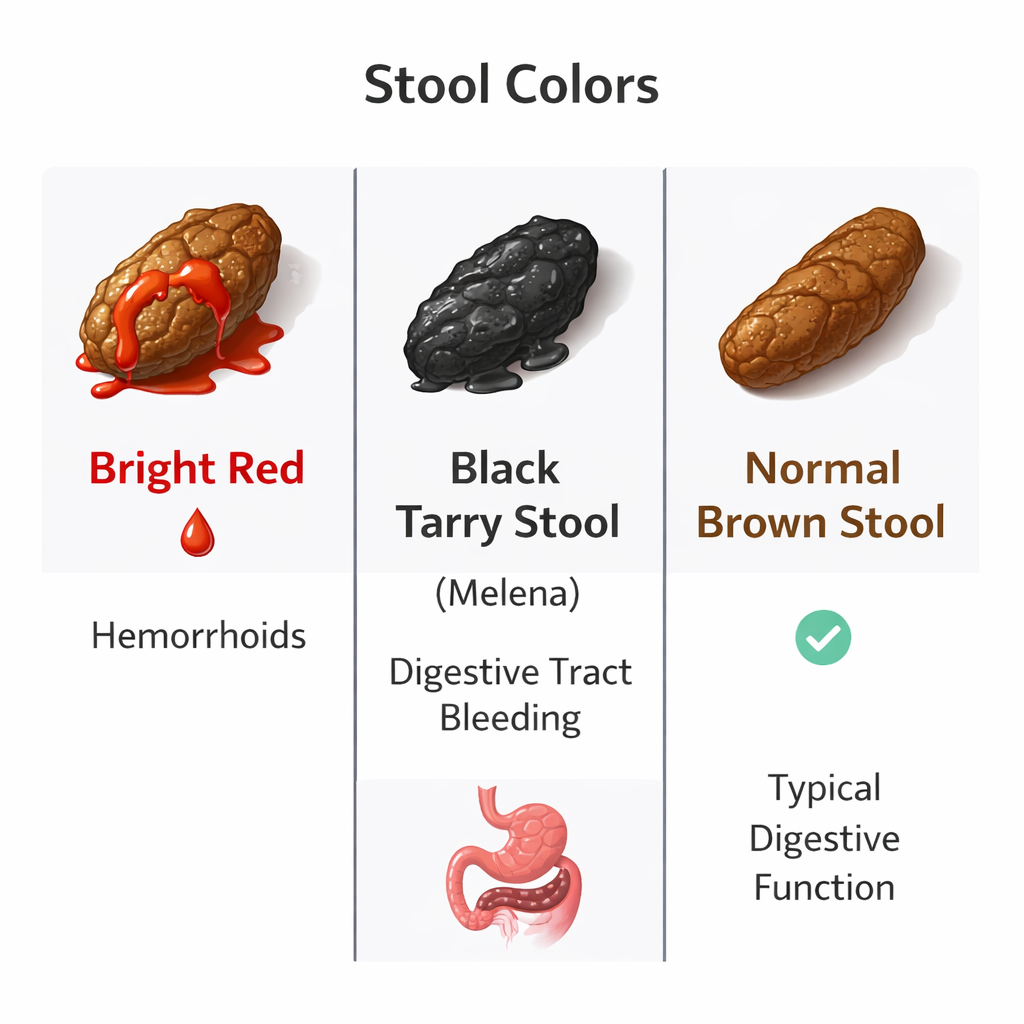
The Bright Red Standard
The hallmark of hemorrhoidal bleeding is bright red blood, medically known as hematochezia when it appears fresh. This occurs because the source of the bleeding is distal (near the end of the digestive tract). The blood has not been exposed to stomach acid or digestive enzymes, which would otherwise darken it.
If you ask, “do hemorrhoids cause blood in stool”, the clinical expectation is:
- Color: Bright red or scarlet.
- Timing: During or immediately after a bowel movement.
- Pain: Internal hemorrhoids often bleed painlessly. External hemorrhoids may bleed if thrombosed (clotted) or irritated, usually accompanied by pain.
Patterns of Bleeding
The location of the blood relative to the stool provides clues about the source.
- On Toilet Paper: This is the most common presentation. You wipe, and the paper is stained with bright red blood. This suggests an anal source, such as hemorrhoids or an anal fissure.
- In the Bowl: Droplets of blood in the toilet water indicate active bleeding from the rectum or anus.
- Coating the Stool: Blood on the outside of the stool suggests the bleeding occurred as the stool passed through the anal canal.
When to Be Concerned About Blood Color
Not all rectal bleeding fits the hemorrhoid profile. If you are asking, “will hemorrhoids cause blood in stool” that looks different, you should pause.
- Dark Red or Maroon: This suggests bleeding may be coming from higher up in the colon (e.g., diverticulosis or colitis).
- Black or Tarry: This is called melena and indicates upper gastrointestinal bleeding (stomach or esophagus). This is not caused by hemorrhoids.
- Mixed In: If the blood appears mixed throughout the stool rather than on the surface, it may indicate inflammation or a lesion higher in the digestive tract.
Mucus and Irritation
In addition to blood, larger hemorrhoids may cause mucus leakage. This can lead to irritation of the surrounding skin, causing itching (pruritus ani) and a sensation of moisture. While not blood, this symptom often accompanies hemorrhoidal bleeding and contributes to the discomfort patients feel.
Clinical Evidence and Guidelines
According to the National Health Service (NHS) and the American Society of Colon and Rectal Surgeons, bright red bleeding is the classic pattern for hemorrhoids. However, they also emphasize that rectal bleeding should never be automatically assumed to be hemorrhoids without ruling out other causes, especially in individuals over the age of 45 or those with a family history of colorectal cancer.
| Bleeding Pattern | More Consistent With | Action Required |
|---|---|---|
| Bright red blood after pooping | Hemorrhoids or anal fissure | Monitor; see doctor if persistent. |
| Red streaks on stool surface | Possible hemorrhoids or lower GI source | Medical evaluation recommended. |
| Dark red or maroon stool | Colon bleeding (e.g., diverticulosis) | See a doctor promptly. |
| Black or tarry stool | Upper GI bleeding (stomach/esophagus) | Seek urgent medical care. |
| Blood mixed inside stool | Inflammation or higher lesion | See a doctor promptly. |
If you are wondering, “can hemorrhoids cause bleeding in the stool”, remember that while they can cause blood to appear with the stool, they do not typically cause the stool itself to become dark or tarry. Understanding this distinction is vital for your safety.
Can Hemorrhoids Cause Thin Stools?
One of the most anxiety-inducing symptoms patients report is a change in stool caliber. Many people search “can hemorrhoids cause thin stools” when they notice their bowel movements appear narrower than usual. This is a critical area where medical clarity is needed to prevent both unnecessary panic and dangerous complacency.
The Clinical Reality
Thin stools are not a classic hallmark of hemorrhoids. While hemorrhoids involve swollen veins in the anal canal, they generally do not narrow the passage enough to consistently change the shape of the stool from normal to thin or pencil-like.
When patients ask, “do hemorrhoids cause thin stools”, the medical consensus is that while large, prolapsing hemorrhoids might create a sensation of fullness or incomplete emptying, they are rarely the structural cause of persistently thin stool. The anal canal is flexible, and hemorrhoidal tissue is soft; it typically compresses rather than rigidly narrows the passage.
Why the Confusion Exists
The confusion arises because both hemorrhoids and more serious conditions (like colorectal cancer) can occur simultaneously. A patient might have hemorrhoids (which are very common) and also develop a polyp or tumor that narrows the colon. If they assume the thin stool is due to the hemorrhoids, they might delay diagnosis of the underlying condition.
When Thin Stool is a Red Flag
If you are asking, “does hemorrhoids cause thin stools”, consider the context. Occasional thin stool can happen due to diet, minor spasms, or temporary constipation. However, persistent thin stools should not be blamed on hemorrhoids alone.
- Persistent Change: If your stool remains thin for more than a few weeks.
- Associated Symptoms: If thin stool is accompanied by bleeding, weight loss, or abdominal pain.
- Age Factor: Individuals over 45 should be particularly cautious.
The “Pencil-Thin” Warning
Medical literature, including guidelines from the Mayo Clinic, notes that skinny or thin stool can happen when a mass narrows the passage in the colon or rectum. While hemorrhoids are located at the very end of the tract, a narrowing higher up will affect the stool shape before it reaches the anus. Therefore, if you are wondering, “will hemorrhoids cause thin stools”, the safer medical assumption is that they do not, and other causes should be investigated.
Internal Hemorrhoids and Stool Shape
Some patients specifically ask, “do internal hemorrhoids cause thin stools”. Internal hemorrhoids are located above the dentate line and are covered by mucosa. Even when enlarged, they rarely obstruct the lumen enough to mold the stool into a thin shape. If you experience consistent narrowing, it suggests a structural issue beyond simple venous swelling.
Can Hemorrhoids Cause Narrow, Skinny, Flat, or Flattened Stools?
Building on the discussion of thin stools, many users search for variations of this symptom using different terms. You might see queries like “can hemorrhoids cause narrow stools”, “can hemorrhoids cause skinny stools”, or “can hemorrhoids cause flat stool”. It is important to address these collectively because they all point to the same concern: a change in stool caliber.
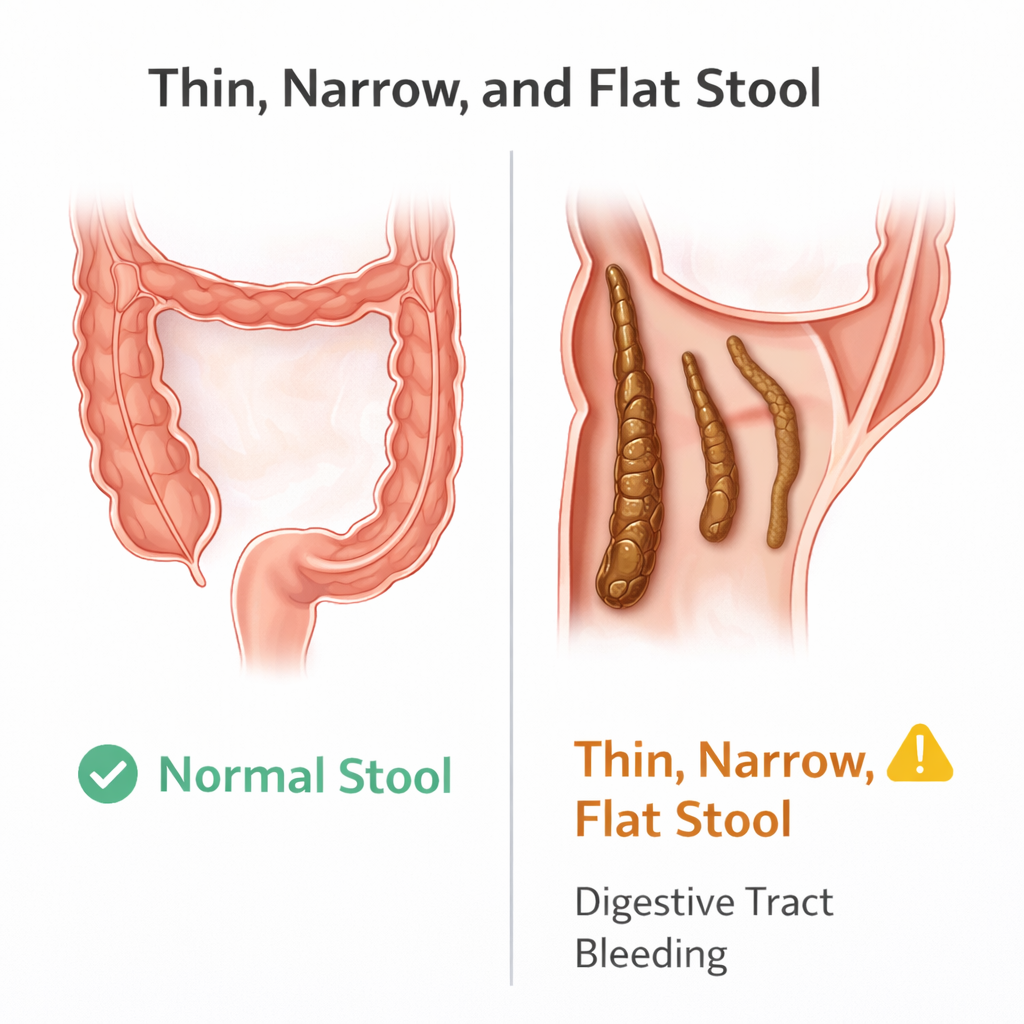
Narrow and Skinny Stools
When people ask, “will hemorrhoids cause narrow stools” or “can hemorrhoids cause narrow stool”, they are describing a reduction in the diameter of the bowel movement. As established, hemorrhoids are not the typical cause of this. A consistent change to narrow or skinny stools suggests that the colon itself may be narrowed.
- Potential Causes: Polyps, tumors, strictures (scar tissue), or inflammation (IBD).
- Hemorrhoid Role: Hemorrhoids might make passing stool uncomfortable, leading to withholding behavior, which can harden stool, but they do not typically mold it into a narrow shape.
Flat or Flattened Stools
Queries like “can hemorrhoids cause flat stool”, “can hemorrhoids cause flat stools”, or “can hemorrhoids cause flattened stool” describe stool that looks ribbon-like or pressed flat. This is often a more specific sign of obstruction.
- Mechanism: For stool to become flat, it usually must pass through a narrowed space that presses it into that shape before it reaches the rectum.
- Hemorrhoid Limitation: Since hemorrhoids are at the exit, they would only affect the shape at the very end of the passage. If the entire stool is flat, the narrowing is likely higher up.
The Importance of Persistence
Occasional changes in stool shape are normal and can be influenced by diet (e.g., low fiber) or hydration. However, persistent changes are the concern.
- Red Flags:
- New persistent thin, narrow, or flat stools.
- Bleeding accompanying the shape change.
- Abdominal pain or cramping.
- Unexplained weight loss.
- Bowel habit changes lasting more than a few days or weeks.
Medical Guidance on Stool Shape
The Mayo Clinic and cancer guidance organizations note that skinny or thin stool can happen when a cancer narrows the passage. Anal cancer guidance also lists thinner stools as a possible symptom, though this is distinct from benign hemorrhoids. Therefore, if you are asking, “can hemorrhoids cause skinny stools”, the answer should be treated with caution. Do not assume it is “just hemorrhoids.” A medical evaluation, potentially including a colonoscopy, is the only way to rule out structural narrowing.
Summary on Stool Shape
- Can hemorrhoids cause narrow stools? Unlikely to be the primary cause.
- Can hemorrhoids cause flat stool? Not typically.
- Action: If stool shape changes persist for more than two weeks, see a doctor regardless of whether you have known hemorrhoids.
Can Hemorrhoids Cause Black Stool?
This is perhaps the most critical safety section of this article. Many users search “can hemorrhoids cause black stool” out of concern after noticing a dark bowel movement. From a medical standpoint, this distinction is vital for your safety.
The Short Answer: No
Usually no. Hemorrhoids typically cause bright red bleeding. Black or tarry stool suggests blood that has been digested, often from higher in the GI tract.
Understanding Melena
Black, tarry, foul-smelling stool is medically known as melena. This occurs when blood originates from the esophagus, stomach, or upper small intestine. As the blood travels through the digestive system, stomach acid and enzymes break down the hemoglobin, turning the blood dark black and giving it a sticky, tar-like consistency.
Why Hemorrhoids Don’t Cause Black Stool
Hemorrhoids are located at the very end of the digestive tract (the anus and lower rectum). Blood from hemorrhoids exits the body almost immediately after bleeding occurs. It does not have time to be digested or darkened. Therefore, if you are asking, “can hemorrhoids cause black stool”, the physiological answer is that it is highly inconsistent with hemorrhoidal bleeding.
When to Seek Urgent Care
If you notice black stool, you should seek medical care promptly. It may suggest gastrointestinal bleeding from higher up in the digestive tract. Conditions that cause black stool include:
- Peptic ulcers.
- Gastritis.
- Esophageal varices.
- Use of certain medications (e.g., iron supplements, bismuth subsalicylate/Pepto-Bismol) which can also darken stool without bleeding.
No, black stool is not a typical hemorrhoid symptom. Hemorrhoids usually cause bright red blood. Black or tarry stool may suggest gastrointestinal bleeding from higher up in the digestive tract and needs medical attention.
Differentiating Food and Medication
Before panicking, consider your recent intake. Iron supplements, blueberries, black licorice, and bismuth-containing medications can turn stool black without indicating bleeding.
However, if you are unsure, or if the stool is tarry and foul-smelling, treat it as a medical priority. If you are wondering, “can hemorrhoids cause black stool”, remember that hemorrhoids are not the culprit for melena. Always err on the side of caution and consult a clinician.
Can Hemorrhoids Cause Loose Stools?
Another common query is “can hemorrhoids cause loose stools”. Patients often wonder if there is a direct causal link between hemorrhoidal disease and diarrhea.
The Relationship Between Hemorrhoids and Diarrhea
Hemorrhoids do not usually directly cause loose stool or diarrhea. The mechanism of hemorrhoids involves swollen veins, which does not inherently alter the consistency of the stool produced by the colon. However, the relationship often works in reverse: diarrhea can irritate hemorrhoids.
How Diarrhea Affects Hemorrhoids
Frequent loose stools can exacerbate existing hemorrhoids. The acidity of liquid stool and the frequency of wiping can lead to:
- Increased inflammation and swelling.
- More significant bleeding due to irritation.
- Heightened pain and itching.
When Loose Stools + Bleeding is Concerning
If you experience loose stools plus rectal bleeding, it may point to other conditions such as:
- Proctitis: Inflammation of the rectal lining.
- Infection: Bacterial or viral gastroenteritis.
- Inflammatory Bowel Disease (IBD): Conditions like Ulcerative Colitis or Crohn’s Disease often present with diarrhea and blood.
Clinical Advice
If you are asking, “can hemorrhoids cause loose stools”, the answer is generally no. If you have persistent diarrhea, especially with blood, you need a evaluation to rule out infection or IBD. Treating it as simple hemorrhoids could delay diagnosis of a more complex gastrointestinal condition.
Internal Hemorrhoids vs External Hemorrhoids — Which One Bleeds More?
Understanding the anatomy of hemorrhoids helps explain the symptoms. When patients ask, “do internal hemorrhoids cause thin stools” or “can hemorrhoids cause blood in the stool”, the type of hemorrhoid matters.
Internal Hemorrhoids
- Location: Inside the rectum, above the dentate line.
- Sensation: Generally painless because there are few pain-sensing nerves in this area.
- Bleeding: Most likely to bleed. Because they are exposed to passing stool, internal hemorrhoids are the primary source of painless, bright red bleeding.
- Prolapse: They can swell and push outside the anus during a bowel movement.
External Hemorrhoids
- Location: Under the skin around the anus.
- Sensation: Painful, itchy, or uncomfortable because this area is rich in nerve endings.
- Bleeding: Less likely to bleed spontaneously unless they are thrombosed (a clot forms inside) or irritated by wiping.
- Appearance: May feel like a lump or swelling around the anus.
Which Bleeds More?
Internal hemorrhoids are the primary culprit for “can hemorrhoids cause bleeding in the stool” scenarios. They are fragile and easily scratched by hard stool. External hemorrhoids are more associated with pain and swelling than significant bleeding. However, large hemorrhoids (whether internal or external) can prolapse and cause mucus leakage, leading to irritation that might result in minor bleeding upon wiping.
What Symptoms Are More Likely to Be Hemorrhoids?
To help you differentiate, here is a breakdown of symptoms that align closely with a hemorrhoid diagnosis. These patterns are supported by NHS symptom lists and clinical guidelines.
Typical Hemorrhoid Symptoms
- Bright red blood after pooping: The most common sign.
- Itching (Pruritus Ani): Irritation around the anal opening.
- A lump around the anus: Feeling of a swelling or tag, especially with external hemorrhoids.
- Discomfort after straining: Pain or pressure during bowel movements.
- Mucus leakage: Moisture or discharge after passing stool.
- Feeling of incomplete emptying: Sensation that you still need to go after finishing.
Context Matters
These symptoms are most likely hemorrhoids if:
- They correlate with constipation or straining.
- The blood is strictly bright red.
- There are no systemic symptoms (like weight loss or fever).
- They improve with home care (fiber, water, topical treatments).
What Symptoms Are Less Likely to Be “Just Hemorrhoids”?
This is a high-value trust section. It is crucial to recognize when symptoms suggest something more serious. Rectal bleeding can overlap with colorectal and anal disease and should not be self-diagnosed.
Red Flag Symptoms
- Black stool: Indicates upper GI bleeding.
- Persistent thin or ribbon-like stool: Suggests structural narrowing.
- Weight loss: Unexplained loss of weight without dieting.
- Fatigue: Could indicate anemia from chronic blood loss.
- Ongoing abdominal pain: Cramping or pain not limited to the anus.
- Bleeding not linked to bowel movements: Spontaneous bleeding.
- Maroon or very dark blood: Suggests higher colon bleeding.
- Symptoms that don’t improve: No change after 1–2 weeks of home care.
The Danger of Assumption
Using Mayo and NHS sources, we stress that rectal bleeding can overlap with colorectal and anal disease. Assuming it is “just hemorrhoids” is a common reason why colorectal cancer diagnoses are delayed in younger adults. If you have these red flags, you need a professional evaluation.
If It’s Not Hemorrhoids, What Else Could Cause Bloody or Thin Stools?
If you are asking “can hemorrhoids cause bloody stools” but your symptoms don’t fit the typical pattern, consider these differential diagnoses. This section helps rank while keeping the article medically responsible.
1. Anal Fissure
A small tear in the lining of the anus.
- Symptoms: Sharp pain during bowel movements, bright red blood.
- Difference: Pain is usually more severe than hemorrhoids.
2. Colorectal Polyps
Growths on the inner lining of the colon.
- Symptoms: Often asymptomatic, but can bleed.
- Risk: Some polyps can become cancerous over time.
3. Colorectal Cancer
A malignant tumor in the colon or rectum.
- Symptoms: Blood in stool (can be dark or bright), change in stool shape (thin/narrow), weight loss, fatigue.
- Importance: Early detection saves lives. Do not ignore persistent changes.
4. Rectal or Anal Cancer
Cancer located in the rectum or anal canal.
- Symptoms: Bleeding, pain, lump, change in bowel habits, thin stools.
5. Diverticulosis
Small pouches that form in the colon wall.
- Symptoms: Can cause significant painless bleeding (often maroon or red).
6. Inflammatory Bowel Disease (IBD)
Includes Crohn’s Disease and Ulcerative Colitis.
- Symptoms: Diarrhea, blood, mucus, abdominal pain, weight loss.
7. Upper GI Bleeding
Ulcers or gastritis.
- Symptoms: Black, tarry stool (melena).
Understanding these possibilities underscores why asking “can hemorrhoids cause bloody stools” is only the first step. A doctor must rule out these other conditions.
When to See a Doctor for Blood in Stool or Thin Stool
Knowing when to seek help is critical. NHS advises rectal bleeding should be checked because it can sometimes be a sign of bowel cancer.

Immediate Medical Attention
- Black stool: Especially if accompanied by dizziness, weakness, or vomiting.
- Heavy bleeding: Soaking through pads or filling the toilet bowl.
- Severe pain: Abdominal or rectal pain that is unbearable.
- Signs of Shock: Lightheadedness, fainting, rapid heartbeat.
Schedule an Appointment Soon
- Any rectal bleeding that is new or unexplained: Even if you think it’s hemorrhoids.
- Thin stool that persists: Lasting more than a week.
- Bowel habit change: Constipation or diarrhea lasting more than a few days.
- Weight loss: Unexplained loss alongside bowel changes.
- Family History: If you have a family history of colorectal cancer, be extra vigilant.
- Age: Individuals over 45 should follow screening guidelines regardless of symptoms.
Don’t Self-Diagnose
While hemorrhoids are common, they are a diagnosis of exclusion. You cannot confirm hemorrhoids without ruling out other causes of bleeding. If you are wondering, “can hemorrhoids cause bloody stools” in your specific case, a doctor can provide the definitive answer.
How Doctors Check Whether It’s Hemorrhoids
If you visit a clinician for these symptoms, what can you expect? Understanding the process can reduce anxiety. NHS notes rectal exams and stool testing may be part of the workup.
1. History and Symptom Pattern
Your doctor will ask about the color of the blood, stool shape, pain levels, diet, and family history. Be honest about your symptoms.
2. Physical Exam
- Visual Inspection: Checking the anus for external hemorrhoids or fissures.
- Digital Rectal Exam (DRE): The doctor inserts a gloved, lubricated finger to feel for abnormalities inside the rectum.
3. Anoscopy or Proctoscopy
A short, rigid tube with a light is inserted into the anus to visualize internal hemorrhoids. This is quick and usually done in the office.
4. Stool Testing
Tests like the FIT (Fecal Immunochemical Test) may be used to detect hidden blood not visible to the eye.
5. Colonoscopy or Specialist Referral
If symptoms are concerning (e.g., thin stool, age over 45, family history), a colonoscopy may be recommended. This allows the doctor to examine the entire colon for polyps, cancer, or inflammation. This is the gold standard for ruling out serious conditions when asking “can hemorrhoids cause bloody stools” vs. something more serious.
Home Care Tips if Hemorrhoids Are the Cause
If your doctor confirms hemorrhoids, or while you are waiting for an appointment, there are evidence-based steps you can take to manage symptoms. NHS-style self-care leaflets commonly emphasize fiber and soft stools.
1. Increase Fiber Intake
- Goal: 25–35 grams of fiber per day.
- Sources: Fruits, vegetables, whole grains, legumes.
- Supplements: Psyllium husk or methylcellulose can help soften stool.
2. Hydration
- Goal: Drink plenty of water throughout the day.
- Why: Fiber needs water to work. Without fluids, fiber can cause constipation.
3. Avoid Straining
- Habits: Do not force bowel movements. If nothing happens, get up and try later.
- Position: Using a footstool to elevate your knees (squatting position) can ease passage.
4. Toilet Habits
- Time: Don’t sit too long on the toilet. Avoid reading or using phones while on the toilet, as this increases pressure on rectal veins.
- Wiping: Use soft, unscented toilet paper or moist wipes (alcohol-free) to reduce irritation.
5. OTC Treatments
- Creams/Suppositories: Hydrocortisone or witch hazel pads can reduce itching and swelling temporarily.
- Pain Relief: Acetaminophen is generally preferred over NSAIDs if bleeding is present, as NSAIDs can thin blood.
6. Seek Care if Symptoms Persist
If home care does not improve symptoms within a week, or if bleeding continues, return to your doctor. Do not assume persistent bleeding is normal.
FAQs
Can hemorrhoids cause bloody stools?
Yes, hemorrhoids are a very common cause of bloody stools, particularly when the blood appears bright red. This occurs because hemorrhoids are swollen veins located in the lower rectum or anus. When strained during a bowel movement, these fragile veins can rupture, leaving blood on toilet paper, dripping into the bowl, or coating the stool surface. However, any new bleeding should be discussed with a provider.
Can hemorrhoids cause blood in stool?
Yes, hemorrhoids can cause blood in stool, but the presentation is specific. The blood is typically found on the exterior surface of the stool or separately in the toilet bowl, rather than being mixed thoroughly inside the fecal matter. If you notice blood mixed within the stool itself, this may indicate a source higher in the digestive tract and requires further medical evaluation to rule out other conditions.
Can hemorrhoids cause blood in the stool?
Similar to other bleeding queries, hemorrhoids cause bleeding that appears with the stool, but it is typically bright red and fresh. This freshness indicates the bleeding source is near the exit point of the digestive system. Darker blood suggests digestion has occurred, pointing away from hemorrhoids. If bleeding persists despite home treatment, or if you feel dizzy, you should seek professional medical advice immediately.
Can hemorrhoids cause thin stools?
Not typically. Persistent thin stools should be evaluated by a doctor to rule out other conditions. While swollen hemorrhoidal tissue might create a sensation of fullness, it rarely physically narrows the canal enough to change stool caliber consistently. Persistent pencil-thin stools can sometimes signal a structural obstruction, such as a polyp or tumor, higher in the colon, necessitating a colonoscopy for accurate diagnosis.
Will hemorrhoids cause narrow stools?
Hemorrhoids are unlikely to cause consistently narrow stools. This symptom warrants medical investigation. Although large prolapsing hemorrhoids can make passing stool feel difficult or obstructed, they do not usually mold the stool into a narrow shape before it exits. If you experience ongoing changes in stool width, especially accompanied by weight loss or pain, please consult a gastroenterologist for proper screening.
Can hemorrhoids cause narrow stool?
While large hemorrhoids might cause a feeling of obstruction, they do not usually mold stool into a narrow shape. The anal canal is flexible, and hemorrhoidal tissue is soft, meaning it compresses rather than rigidly narrowing the passage. Consistent narrow stool often suggests a fixed narrowing elsewhere in the colon. Therefore, assuming this symptom is solely due to hemorrhoids could delay the diagnosis of more serious gastrointestinal issues.
Can hemorrhoids cause skinny stools?
Skinny stools are not a classic symptom of hemorrhoids and may indicate a narrowing higher in the colon. Many patients worry when they see pencil-thin movements, and rightly so. While occasional changes happen due to diet or spasms, persistent skinny stools combined with bleeding or fatigue are red flags. It is crucial not to self-diagnose hemorrhoids without a professional exam to exclude colorectal cancer or other structural diseases.
Can hemorrhoids cause flat stool?
Flat or ribbon-like stool is not typical for hemorrhoids and should be checked by a clinician. This shape often implies that the stool is being pressed into a specific form as it moves through a narrowed section of the bowel. Since hemorrhoids are located at the very end of the tract, they cannot shape the stool throughout its length. Persistent changes in shape require diagnostic imaging or endoscopy.
Can hemorrhoids cause black stool?
No. Black stool suggests upper gastrointestinal bleeding and is not caused by hemorrhoids. Seek medical attention. Black, tarry stool, known medically as melena, indicates blood has been digested by stomach acid, pointing to issues like ulcers in the stomach or esophagus. Hemorrhoids produce fresh, red blood. If you observe black stools, especially with weakness or vomiting, go to the emergency room, as this indicates a potentially serious internal bleeding event.
Can hemorrhoids cause loose stools?
Hemorrhoids do not cause diarrhea, but diarrhea can irritate hemorrhoids and worsen symptoms. The relationship is usually reverse; frequent loose stools increase wiping and acidity around the anus, inflaming existing hemorrhoids. However, if you experience loose stools accompanied by blood, it could indicate inflammatory bowel disease or infection rather than simple hemorrhoids. Tracking your bowel habits and reporting changes to your doctor helps ensure accurate treatment.
Do internal hemorrhoids cause thin stools?
Internal hemorrhoids typically cause painless bleeding. They are not a common cause of thin stool shape changes. Located above the pain-sensitive dentate line, internal hemorrhoids often bleed without warning during straining. However, they lack the structural rigidity to compress stool into a thin form consistently. If you have internal hemorrhoids and notice shape changes, do not assume they are linked. A full colorectal evaluation is needed to ensure safety.
Final Medical Thoughts
Navigating symptoms like bloody stools, thin stools, or black stool can be stressful. While hemorrhoids are a very common and often benign explanation for bright red bleeding, they are not the only explanation. As a physician, my advice is to never ignore persistent changes in your bowel habits.
If you are asking “can hemorrhoids cause bloody stools”, know that while they can, the context matters. Bright red blood is reassuring, but black stool, thin stool, or bleeding accompanied by weight loss requires prompt medical evaluation. Early detection of gastrointestinal conditions is key to successful treatment. Prioritize your health, consult a professional, and do not rely solely on internet searches for diagnosis.
References:
https://www.mayoclinic.org/diseases-conditions/hemorrhoids/symptoms-causes/syc-20360268
https://www.nhs.uk/symptoms/bleeding-from-the-bottom-rectal-bleeding/
https://www.nhs.uk/conditions/piles-haemorrhoids/
https://www.mayoclinic.org/symptoms/rectal-bleeding/basics/definition/sym-20050740
https://www.mayoclinic.org/symptoms/rectal-bleeding/basics/causes/sym-20050740
https://www.nidirect.gov.uk/conditions/rectal-bleeding
https://www.mayoclinic.org/diseases-conditions/gastrointestinal-bleeding/symptoms-causes/syc-20372729
https://www.mayoclinic.org/diseases-conditions/diarrhea/expert-answers/stool-color/faq-20058080
https://www.mayoclinic.org/diseases-conditions/irritable-bowel-syndrome/expert-answers/narrow-stools/faq-20057781
https://www.mayoclinic.org/diseases-conditions/colon-cancer/in-depth/colon-cancer-stool/art-20586915
https://www.mayoclinic.org/medical-professionals/digestive-diseases/news/hemorrhoidal-disease-diagnosis-and-management/mac-20430067






