If you’re scheduled for a prostate biopsy, you may be wondering, ‘What are the chances that it will detect cancer?’ This is a common concern for many men facing the procedure. A prostate biopsy is one of the primary methods used to diagnose prostate cancer, and it plays a critical role in determining the appropriate treatment plan. Given the prevalence of prostate cancer, many men are understandably anxious about the results.
In this article, we will explore what percentage of prostate biopsies are cancerous, what this statistic means, and the factors that may influence the results. Understanding these odds can help alleviate anxiety and provide clarity on the next steps in your healthcare journey.
What Is a Prostate Biopsy?
A prostate biopsy is a medical procedure in which a small sample of tissue is taken from the prostate gland to examine for signs of cancer or other prostate conditions. It is commonly used to diagnose prostate cancer in men who have elevated Prostate-Specific Antigen (PSA) levels or abnormal findings from a digital rectal exam (DRE). A biopsy is necessary to confirm whether prostate cancer is present and determine its aggressiveness.
There are several types of prostate biopsies, with the two most common being:
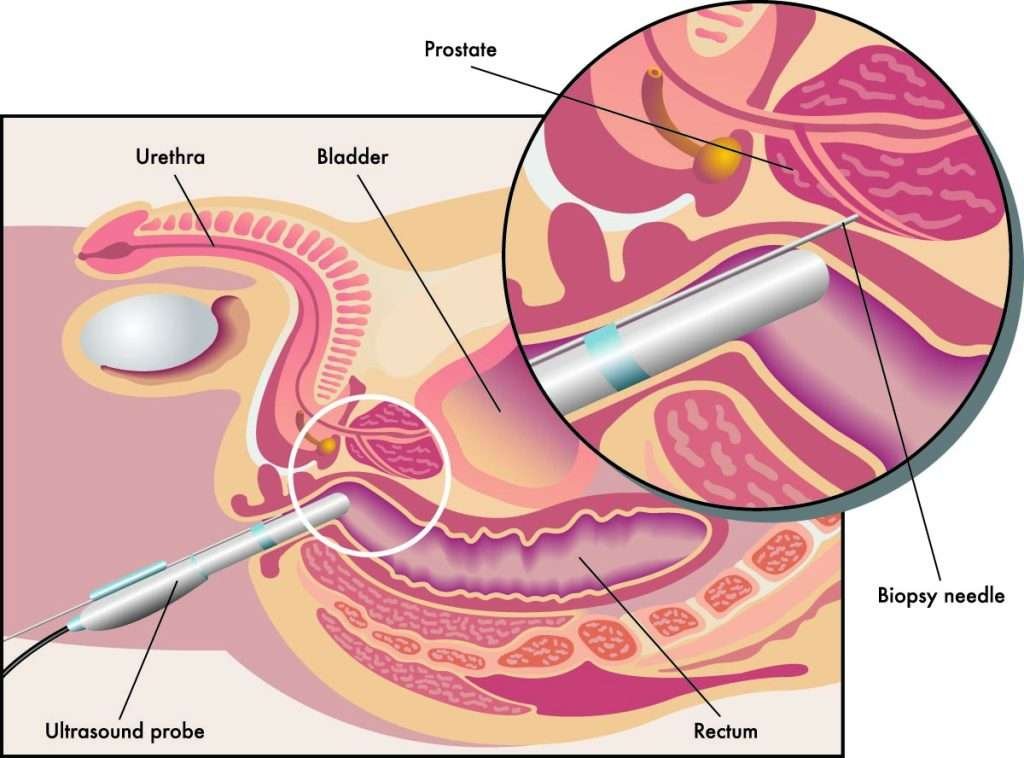
- Transrectal Ultrasound-Guided Biopsy (TRUS): The most frequently used method, where a small ultrasound probe is inserted into the rectum to guide a needle into the prostate to collect tissue samples.
- Transperineal Biopsy: A less common method where the biopsy needle is inserted through the skin between the scrotum and anus, often used in specific cases when TRUS is not ideal.
A prostate biopsy is typically recommended when there are abnormal signs, such as elevated PSA levels or abnormal findings from a DRE. These tests alone cannot confirm the presence of cancer, and a biopsy provides a definitive diagnosis, allowing doctors to determine the best course of treatment.
How Are Prostate Biopsies Performed?
A prostate biopsy is typically performed in a healthcare setting, often on an outpatient basis. The procedure begins with the patient being positioned on their side or back, depending on the biopsy method used. A local anesthetic is administered to numb the area, and in some cases, a sedative may be given to help the patient relax. The doctor uses an ultrasound or other imaging techniques to guide a thin, hollow needle into the prostate, collecting small tissue samples from various areas of the gland.
Patients can expect to experience minimal discomfort during the procedure, though some pressure or mild discomfort may occur. The procedure usually takes about 10 to 20 minutes. Afterward, patients may experience mild soreness or bruising in the biopsy area, as well as some blood in the urine, stool, or semen for a short period. It is important to follow post-procedure instructions to reduce the risk of complications, such as infection or excessive bleeding.
While prostate biopsies are generally reliable, there are risks of false positives (when cancer is detected but it’s not actually present) and false negatives (when cancer is missed). The accuracy of the biopsy depends on factors such as the number of samples taken, the biopsy technique, and the skill of the practitioner. A higher number of tissue samples typically improves accuracy, as prostate cancer can be localized to certain areas.
What Percentage of Prostate Biopsies Are Cancerous?
Prostate biopsies typically return positive for cancer in about 20-30% of cases, though this percentage can vary based on several factors. The likelihood of a biopsy showing cancer depends on the patient’s age, PSA levels, and other individual risk factors.
Key factors influencing biopsy results:
- PSA Levels: Men with elevated PSA levels have a higher chance of a positive biopsy. For instance, men with PSA levels above 10 ng/mL are more likely to have prostate cancer detected on biopsy.
- Age: The risk of prostate cancer increases with age, so older men are more likely to have a positive biopsy.
- Family History: A family history of prostate cancer can significantly increase the likelihood of a positive result, as genetics play a role in the disease’s development.
- Abnormal Digital Rectal Exam (DRE): Abnormalities detected during a DRE, such as an irregular or hard prostate, can lead to a higher probability of cancer being found on biopsy.
It’s also essential to consider the risk of overdiagnosis, particularly in older men. Some low-grade prostate cancers may not impact life expectancy or require aggressive treatment, leading to unnecessary interventions. Therefore, the decision to perform a prostate biopsy should involve a comprehensive discussion between the patient and the healthcare provider to weigh the risks and benefits carefully.
What Does a Positive Biopsy Result Mean?
A positive prostate biopsy result means that cancer cells have been detected in the prostate tissue sample. After a diagnosis, staging and grading are essential steps in understanding the cancer’s severity and aggressiveness.
- Staging refers to determining how far the cancer has spread, whether it’s confined to the prostate (localized) or if it has spread to nearby tissues or distant organs (advanced).
- Grading evaluates the aggressiveness of the cancer. The Gleason score is commonly used, with a higher score indicating a more aggressive cancer. This score is based on the patterns of the cancerous cells seen under the microscope, guiding treatment decisions.

Following a positive biopsy, the next steps usually include:
- Further Testing: Additional tests, such as imaging (e.g., MRI, bone scans), may be recommended to assess the cancer’s spread or help in staging.
- Treatment Options: Depending on the stage and grade, treatment options may include active surveillance (for slow-growing cancers), surgery (prostatectomy), radiation therapy, or hormone therapy. Some men may also consider focal treatments if the cancer is localized.
- Discussions with Healthcare Providers: It’s crucial to discuss treatment options thoroughly with oncologists to determine the best course of action based on the patient’s overall health, cancer characteristics, and preferences.
The emotional impact of a cancer diagnosis can be significant, and it’s important to acknowledge feelings of fear, anxiety, or uncertainty. Seeking support from family, friends, or counseling can help manage these emotions, and support groups or professional guidance can provide additional coping strategies. Understanding the diagnosis and having a treatment plan can empower patients and their families to move forward confidently.
What If the Biopsy Result Is Negative?
A negative biopsy result means that no cancer was found in the tissue samples taken from the prostate. However, this does not necessarily rule out cancer. Biopsy results can sometimes miss cancerous tissue, especially if the cancer is small or located in areas that were not sampled. Additionally, prostate cancer can be slow-growing, and some cancers may not be detectable in the early stages.
Further Monitoring may be necessary if a patient continues to experience symptoms like elevated PSA levels or abnormal digital rectal exam findings. In such cases, additional tests might be recommended, including:
- Repeat Biopsy: If symptoms persist or risk factors remain high, another biopsy may be needed.
- MRI or Other Imaging: Advanced imaging techniques can provide a clearer view of the prostate and help identify suspicious areas that may not have been sampled in the biopsy.
- Active Surveillance: For patients with ongoing concerns but no cancer found, active surveillance may be an option. This involves monitoring PSA levels, conducting regular exams, and imaging as necessary.
After a negative result, the next steps typically include:
- Regular Check-ups: Ongoing visits to a healthcare provider to monitor health.
- Monitoring PSA Levels: Continued tracking of PSA levels to detect any changes that could indicate a potential issue.
- Healthy Lifestyle: Maintaining a balanced diet, regular exercise, and stress management to support prostate health.
Although a negative result is reassuring, patients should remain vigilant and proactive about their health, discussing any concerns with their doctor.
Factors Influencing the Results of a Prostate Biopsy
Several factors can influence the outcome of a prostate biopsy, affecting the likelihood of detecting cancer and the accuracy of the results.
Age and Family History:
Age is a significant factor in prostate cancer risk, with the likelihood of developing the disease increasing with age. Men over 50, especially those with a family history of prostate cancer, are at higher risk, which may lead to a higher chance of a positive biopsy result. Family history, particularly a history of first-degree relatives with prostate cancer, significantly raises the risk and may prompt earlier or more frequent biopsies.
PSA Levels:

Prostate-specific antigen (PSA) levels are an essential tool in evaluating prostate cancer risk. Elevated PSA levels can indicate the presence of prostate cancer, though they can also be influenced by other conditions like benign prostatic hyperplasia (BPH). A higher PSA level often increases the likelihood of a positive biopsy result, but it’s not definitive, and PSA levels can vary based on individual health factors. Some men with high PSA levels may have negative biopsy results, while others with normal PSA levels may still have prostate cancer.
Biopsy Technique and Number of Samples:
The method of biopsy, such as transrectal ultrasound-guided biopsy or transperineal biopsy, can affect the accuracy of the results. Transrectal biopsies, commonly used, may have a lower detection rate for cancers located in the anterior (front) part of the prostate. The number of tissue samples taken is also crucial; typically, 10-12 samples are collected, but fewer samples may result in missed diagnoses. More extensive sampling improves detection rates, but it can also increase complications.
Other Health Conditions:
Conditions like benign prostatic hyperplasia (BPH) can complicate biopsy results. BPH causes prostate enlargement, leading to increased PSA levels and potential difficulty in obtaining accurate tissue samples, sometimes resulting in false negatives. Other conditions, like prostatitis or urinary tract infections, can also affect the biopsy outcome.
Frequently Asked Questions
1. What are the chances of a prostate biopsy being positive for cancer?
The chances of a prostate biopsy being positive for cancer typically range from 20-30%, depending on factors like age, PSA levels, family history, and the presence of abnormal findings during a digital rectal exam (DRE).
2. Can a negative biopsy result still mean I have prostate cancer?
Yes, a negative biopsy does not completely rule out prostate cancer, as the procedure can sometimes miss cancerous tissue, especially if the cancer is located in areas not sampled.
3. How accurate are prostate biopsies?
Prostate biopsies are generally accurate, but their accuracy depends on factors such as the number of tissue samples taken, the biopsy technique used, and PSA levels. False positives and false negatives can occur, so additional testing may sometimes be needed.
4. Does a positive biopsy always mean I need treatment?
Not necessarily. A positive biopsy indicates the presence of cancer, but treatment decisions depend on factors such as the cancer’s grade, stage, and whether it is likely to grow aggressively. Active surveillance may be recommended for low-risk cancers.
5. Can the biopsy miss prostate cancer?
Yes, prostate biopsies can miss cancer, especially if the cancer is in a less accessible part of the prostate or if insufficient tissue samples are taken. Further testing or repeat biopsies may be needed in some cases.
Conclusion
Prostate biopsies play a critical role in diagnosing prostate cancer, but the likelihood of a positive result varies based on factors such as age, PSA levels, family history, and biopsy technique. While roughly 20-30% of biopsies return positive for cancer, a negative result does not fully rule out the possibility of prostate cancer, as biopsies can miss cancerous tissue. Understanding the implications of biopsy results and discussing them with your healthcare provider is essential for determining the next steps, whether it be further testing, active surveillance, or treatment options.
If you’ve had a prostate biopsy, it’s important to seek support from healthcare providers and ask questions to fully comprehend the results, the accuracy of the biopsy, and the recommended course of action. By engaging in open communication with your doctor, you can make informed decisions about your prostate health and the appropriate steps to take moving forward.