Introduction
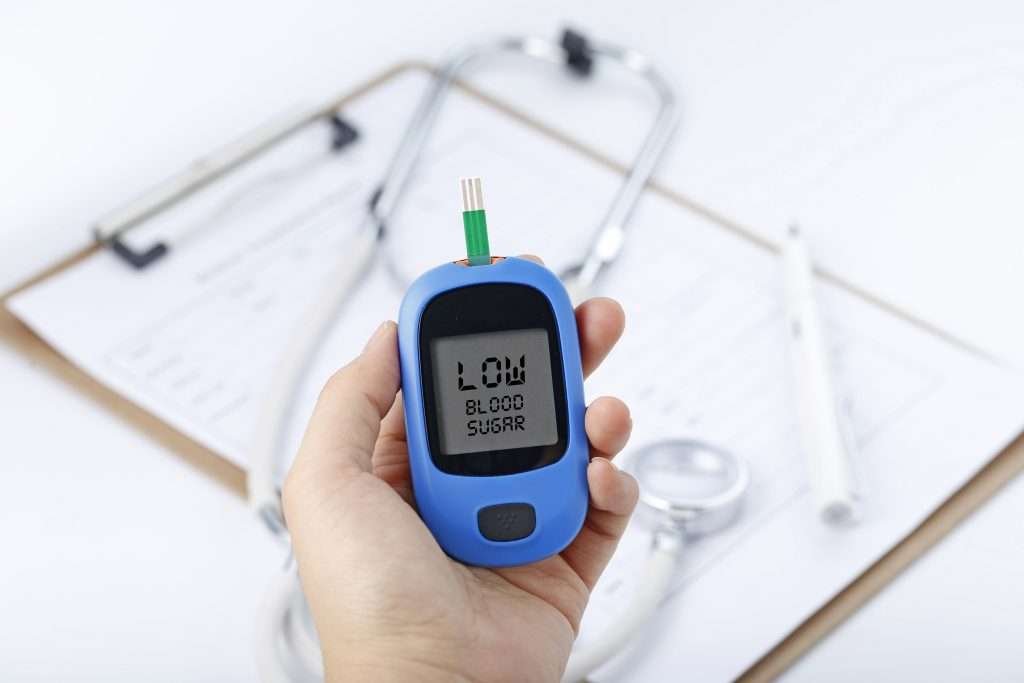
Managing diabetes can often feel like balancing on a tightrope, especially when it comes to preventing low blood sugar episodes. Nighttime hypoglycemia, or low blood sugar at night, occurs when blood glucose levels drop below the normal range (typically below 70 mg/dL) while you’re asleep. This can be a frightening and potentially dangerous experience for anyone managing diabetes.
Understanding how to deal with low blood sugar at night is essential for maintaining your overall health and ensuring a good night’s rest. Nighttime hypoglycemia often goes unnoticed until symptoms disrupt sleep or result in dangerous lows. This makes it crucial to identify the causes, recognize the warning signs, and know what steps to take if it happens.
Ignoring nighttime hypoglycemia can lead to severe consequences, such as seizures, diabetic coma, or even heart complications. Additionally, the lack of restful sleep can affect your energy, mood, and blood sugar control the next day. By learning how to prevent and manage low blood sugar at night, you can reduce these risks and improve your quality of life. Let’s dive deeper into what nighttime hypoglycemia is and how it impacts individuals with diabetes.
What is Nighttime Hypoglycemia?
Nighttime hypoglycemia, also known as nocturnal hypoglycemia, refers to episodes of low blood sugar that occur during sleep. Blood sugar is considered low when it drops below 70 mg/dL, though symptoms and thresholds may vary among individuals.
For people living with diabetes—whether Type 1 or Type 2—nighttime hypoglycemia can present unique challenges. While our bodies naturally regulate blood sugar levels, individuals on insulin therapy or glucose-lowering medications are more prone to nighttime lows. This is because these treatments can sometimes lower blood sugar levels beyond the intended range, especially during periods of inactivity like sleep.
Experiencing low blood sugar at night not only disrupts glucose stability but also increases health risks. Symptoms such as night sweats, trembling, vivid dreams, or sudden awakenings can leave you feeling fatigued and disoriented. Over time, frequent nighttime hypoglycemia can impact your overall health by increasing the likelihood of severe complications, disrupting sleep patterns, and making blood sugar levels harder to manage.
Understanding how to deal with low blood sugar at night starts with awareness. Recognizing the risks and triggers of nocturnal hypoglycemia is the first step in developing an effective prevention and management strategy. With the right knowledge and tools, it’s possible to regain control and sleep soundly.
Symptoms of Low Blood Sugar at Night

Recognizing the symptoms of low blood sugar at night is crucial for taking quick action and preventing severe complications. Nighttime hypoglycemia can occur without warning, but it often manifests through several common symptoms:
- Night sweats: Waking up drenched in sweat, even if the room isn’t hot, can signal a significant drop in blood sugar levels.
- Shaking, trembling, or dizziness: These are physical signs that your body is trying to compensate for low glucose levels.
- Rapid heartbeat: A racing or irregular heartbeat during sleep might indicate a hypoglycemic episode.
- Vivid dreams or nightmares: Unusually intense or frightening dreams are often linked to a drop in blood sugar during REM sleep.
- Weakness or hunger upon waking: Feeling unusually weak, lightheaded, or extremely hungry when you wake up may be a sign of overnight hypoglycemia.
If you’re learning how to deal with low blood sugar at night, understanding these symptoms can make all the difference. Early recognition allows you to treat the condition before it escalates into something more severe, such as a seizure or diabetic coma.
These symptoms can disrupt your sleep and leave you feeling drained the next day. For people managing diabetes, identifying these warning signs is the first step toward maintaining safe blood sugar levels overnight and reducing the risk of complications.
Causes of Nighttime Hypoglycemia
Understanding the causes of low blood sugar at night is essential for preventing it. Several factors can trigger nighttime hypoglycemia, each with unique scenarios that make the condition challenging to manage.
- Excessive insulin before bed
Taking too much insulin at night, especially long-acting or basal insulin, can lower blood sugar levels too much while you sleep. For example, if you miscalculate your insulin dose after dinner, your blood sugar may dip dangerously low by midnight. Adjusting insulin doses with your doctor’s guidance is a key aspect of learning how to deal with low blood sugar at night. - Skipping meals or eating insufficient carbohydrates
Skipping dinner or eating a carb-light meal before bed can lead to glucose depletion overnight. Your body continues to use energy while you sleep, and without enough carbs to sustain you, blood sugar levels may drop too low. - High alcohol consumption
Drinking alcohol, particularly in the evening, can interfere with your liver’s ability to release stored glucose. For example, having a few drinks at a party without eating afterward can set the stage for nighttime hypoglycemia. - Increased physical activity during the day
Intense exercise earlier in the day can make your muscles use more glucose, which can lower blood sugar levels hours later, even while you’re sleeping. For instance, a long hike or workout without adjusting your meals or insulin can result in nighttime blood sugar dips. - Hormonal changes
During sleep, the body naturally produces less of certain counter-regulatory hormones like cortisol and glucagon, which help prevent blood sugar from dropping too low. This hormonal shift can make you more susceptible to nocturnal hypoglycemia.
When figuring out how to deal with low blood sugar at night, it’s vital to identify which of these factors might be contributing to your experience. By addressing these causes, you can take proactive steps to stabilize blood sugar levels and minimize risks. Whether it’s adjusting insulin doses, eating a balanced bedtime snack, or avoiding late-night alcohol, small changes can lead to better sleep and improved health.
Immediate Remedies for Low Blood Sugar at Night
Knowing how to deal with low blood sugar at night is essential for preventing serious complications. If you wake up feeling the symptoms of nighttime hypoglycemia, follow these steps immediately to stabilize your blood sugar levels.
- Check Your Blood Sugar
The first step is to confirm the hypoglycemia. Use your glucometer or Continuous Glucose Monitor (CGM) to check your blood sugar levels. If they are below 70 mg/dL, quick action is necessary to bring them back to a safe range. - Apply the 15-15 Rule
The “15-15 rule” is a proven strategy for managing low blood sugar:- Consume 15 grams of fast-acting carbohydrates.
- Wait 15 minutes and recheck your blood sugar levels.
- Repeat if necessary until your blood sugar stabilizes above 70 mg/dL.
- Quick Fixes for Immediate Relief
Fast-acting carbs can quickly raise blood sugar levels. Keep these items near your bed for convenience:- Glucose tablets or gels: These are highly effective and easy to measure.
- Fruit juice or honey: A small glass of juice or a tablespoon of honey works quickly.
- Small snacks like crackers or candy: These are helpful when glucose-specific products aren’t available.
These remedies are crucial when learning how to deal with low blood sugar at night because they provide the immediate energy your body needs to recover.
- Using Glucagon for Severe Cases
If your blood sugar drops so low that you’re unable to consume carbohydrates—or if you lose consciousness—glucagon may be necessary. A glucagon injection or nasal spray is a life-saving treatment that helps raise blood sugar levels rapidly. It’s essential to educate family members or caregivers on how to use glucagon so they can assist in emergencies. - Keep Emergency Supplies by Your Bed
Preparation is key to managing nighttime hypoglycemia. Always keep a “low blood sugar kit” by your bedside, including:- A glucometer or CGM.
- Glucose tablets or gels.
- A small bottle of juice or a packet of honey.
- Emergency snacks like crackers or candy.
- A glucagon kit for severe cases.
Being prepared ensures you can respond quickly, even if you’re groggy or disoriented.
Understanding how to deal with low blood sugar at night involves both immediate action and long-term planning. These remedies not only stabilize blood sugar levels but also provide peace of mind, helping you sleep safely and soundly.
How to Prevent Low Blood Sugar at Night

Prevention is the cornerstone of managing nighttime hypoglycemia. Taking proactive steps to maintain stable blood sugar levels during sleep can greatly reduce the risk of nocturnal lows. By following these tips, you’ll master how to deal with low blood sugar at night and enjoy a restful, worry-free sleep.
1. Eat a Balanced Bedtime Snack
Choosing the right bedtime snack is essential for keeping blood sugar stable overnight. Snacks that combine carbohydrates with protein are particularly effective, as the carbs provide an immediate glucose boost while the protein helps sustain those levels for longer. Here are some excellent options:
- Peanut butter and crackers: The carbs in crackers and the protein in peanut butter work together to stabilize blood sugar.
- Greek yogurt with berries: Low in sugar but rich in protein, this snack offers sustained energy.
- Apple slices with cheese: A mix of natural sugar, fiber, and protein to keep blood sugar steady overnight.
By including snacks like these in your routine, you’ll be better equipped to prevent nighttime hypoglycemia.
2. Adjust Insulin Dosage with Your Healthcare Provider
If you’re frequently experiencing low blood sugar at night, it’s critical to reassess your insulin dosage. Speak with your doctor or diabetes educator to fine-tune your basal insulin levels or meal-time doses. This ensures you’re not taking more insulin than your body needs, especially before bed. Tailored adjustments are a vital component of learning how to deal with low blood sugar at night.
3. Monitor Blood Sugar Before Bed
Checking your blood sugar levels before sleep is a must. Aim for a safe range (typically between 100-140 mg/dL, though this may vary based on individual circumstances). If your blood sugar is on the lower side, consider having a small snack to prevent dips during the night. Regular pre-bed monitoring helps you identify trends and adjust your routine accordingly.
4. Use Continuous Glucose Monitors (CGMs)
CGMs are game-changers for managing diabetes, especially at night. These devices track blood sugar levels in real time and alert you if levels drop too low. Some even have automatic shutoff features for insulin pumps, adding an extra layer of safety. Incorporating CGM technology is a powerful way to stay ahead when figuring out how to deal with low blood sugar at night.
5. Minimize Alcohol or Pair It with Food
Alcohol can lower blood sugar levels by interfering with the liver’s ability to release stored glucose. To reduce this risk, limit alcohol intake, especially in the evening. If you do drink, pair it with food to help buffer potential drops in blood sugar. For example, enjoying a small snack with your drink can go a long way in preventing nighttime lows.
Creating a Personalized Prevention Plan
To effectively prevent low blood sugar at night, it’s helpful to create a tailored plan based on your lifestyle and diabetes management needs. Here’s how:
- Track Your Patterns: Keep a log of your nighttime blood sugar readings, insulin doses, meals, and activities. Look for patterns that might lead to nighttime hypoglycemia.
- Incorporate Safety Measures: Set alarms for mid-night glucose checks if you’re prone to hypoglycemia.
- Collaborate with Your Healthcare Team: Regularly review your data with your doctor or diabetes educator to make necessary adjustments to your medication, diet, or exercise routine.
By implementing these preventive strategies, you’ll gain better control over your blood sugar levels and significantly reduce the likelihood of nighttime hypoglycemia. Knowing how to deal with low blood sugar at night is not just about addressing the symptoms when they happen—it’s about taking steps to stop them from happening in the first place. With preparation, monitoring, and a little planning, you can sleep soundly, confident in your ability to maintain stable glucose levels.
How Nighttime Hypoglycemia Impacts Your Health
Untreated nighttime hypoglycemia can have serious long-term consequences, affecting both your physical health and overall quality of life. Beyond the immediate danger of dangerously low blood sugar, these episodes can lead to chronic issues that disrupt daily routines and long-term diabetes management.
One of the most immediate effects is poor quality of sleep. Frequent awakenings caused by symptoms like night sweats, rapid heartbeat, or vivid nightmares can leave you feeling fatigued and unfocused during the day. Over time, this lack of restorative sleep can impact your energy levels, mental health, and productivity.
Additionally, repeated episodes of low blood sugar at night increase the risk of seizures or severe hypoglycemia, which can escalate to a diabetic coma if left unaddressed. This is particularly concerning for individuals who live alone or do not have a support system to assist during emergencies.
Nighttime lows can also negatively affect daytime blood sugar control, as the body may overcompensate for overnight drops. This can lead to rebound hyperglycemia (high blood sugar) or make glucose management more unpredictable.
Understanding how to deal with low blood sugar at night is essential for maintaining overall health stability. By addressing the root causes and managing symptoms promptly, you can protect your long-term health and improve your daily life.
When to Seek Medical Advice
While self-management is often effective, there are times when professional help is necessary to manage nighttime hypoglycemia. If you’re experiencing frequent episodes or find that your prevention strategies aren’t working, it’s time to reach out to your diabetes care team.
Frequent Nighttime Episodes: If low blood sugar at night occurs multiple times per week, it could indicate an underlying issue with your treatment plan, such as an incorrect insulin dose or medication mismatch.
Ineffective Self-Management: Despite adjusting snacks, insulin, or routines, some individuals may still struggle with nighttime lows. This could signal a need for more advanced interventions, such as medication adjustments or the use of a Continuous Glucose Monitor (CGM).
Concerns About Insulin or Medication: If you suspect your medication or insulin regimen is contributing to nighttime hypoglycemia, your healthcare provider can help fine-tune your treatment plan.
The role of your diabetes care team is critical for long-term success. They can provide personalized recommendations, troubleshoot issues, and offer support to help you manage nighttime hypoglycemia effectively.
Conclusion
Managing nighttime hypoglycemia is a key part of overall diabetes care. From recognizing symptoms like night sweats and vivid dreams to applying immediate remedies like the 15-15 rule, understanding how to deal with low blood sugar at night can save you from dangerous complications and sleepless nights.
Prevention is just as important as treatment. Eating balanced bedtime snacks, monitoring blood sugar levels, and consulting with your doctor about insulin dosages can help stabilize glucose levels overnight. Using tools like Continuous Glucose Monitors (CGMs) provides added security by alerting you to drops in blood sugar before they become severe.
If you experience frequent nighttime episodes or struggle to control them despite your best efforts, don’t hesitate to seek professional advice. Your diabetes care team is there to guide you toward solutions tailored to your needs.
By staying prepared, self-monitoring regularly, and maintaining open communication with healthcare providers, you can effectively manage nighttime hypoglycemia and improve your overall well-being. With consistent effort, restful nights and stable blood sugar levels are well within reach.
FAQ: How to Deal with Low Blood Sugar at Night
1. What is low blood sugar at night, and how common is it?
Low blood sugar at night, or nighttime hypoglycemia, occurs when blood glucose levels drop below 70 mg/dL during sleep. It’s common in individuals with diabetes, especially those on insulin or glucose-lowering medications.
2. What are the main symptoms of low blood sugar at night?
Symptoms include night sweats, rapid heartbeat, shaking, vivid dreams, or waking up feeling weak or hungry. Recognizing these signs early is vital.
3. How can I quickly treat low blood sugar at night?
Follow the 15-15 rule: consume 15 grams of fast-acting carbs (e.g., glucose tablets, juice, or honey), wait 15 minutes, and recheck your levels.
4. How can I prevent nighttime hypoglycemia?
Eat a balanced bedtime snack, monitor blood sugar before sleep, and work with your doctor to adjust insulin or medication.
5. When should I see a doctor?
Seek medical advice if nighttime episodes are frequent or self-management isn’t effective.





