Can a procedure commonly used for bladder conditions also detect prostate cancer? While cystoscopy is primarily known for diagnosing bladder and urethral issues, its role in detecting prostate cancer is often overlooked. Cystoscopy involves inserting a thin tube with a camera into the bladder to examine the urinary tract, but its potential for detecting prostate cancer is still a subject of discussion.
In prostate cancer diagnosis, early detection plays a key role in treatment success. While cystoscopy isn’t typically used for this purpose, understanding its limitations and the circumstances under which it may be helpful is crucial.
Can a cystoscopy detect prostate cancer? This article will explore how cystoscopy works, when it might be used in conjunction with other tests for prostate cancer, and discuss alternative diagnostic methods that play a more central role in early detection of the disease. By the end of this article, readers will have a clearer understanding of cystoscopy’s role in prostate cancer diagnosis and the best practices for early detection.
What is a Cystoscopy?
A cystoscopy is a diagnostic procedure where a thin, flexible tube called a cystoscope, equipped with a camera, is inserted through the urethra to examine the bladder and urinary tract. This allows doctors to directly view the bladder lining, urethra, and surrounding structures to identify any abnormalities or signs of disease.
Typically, cystoscopy is used to diagnose a variety of conditions affecting the bladder and urethra, such as bladder infections, urinary tract infections (UTIs), bladder cancer, kidney stones, and urethral strictures. It can also help investigate causes of frequent urination, blood in the urine, or pain during urination.
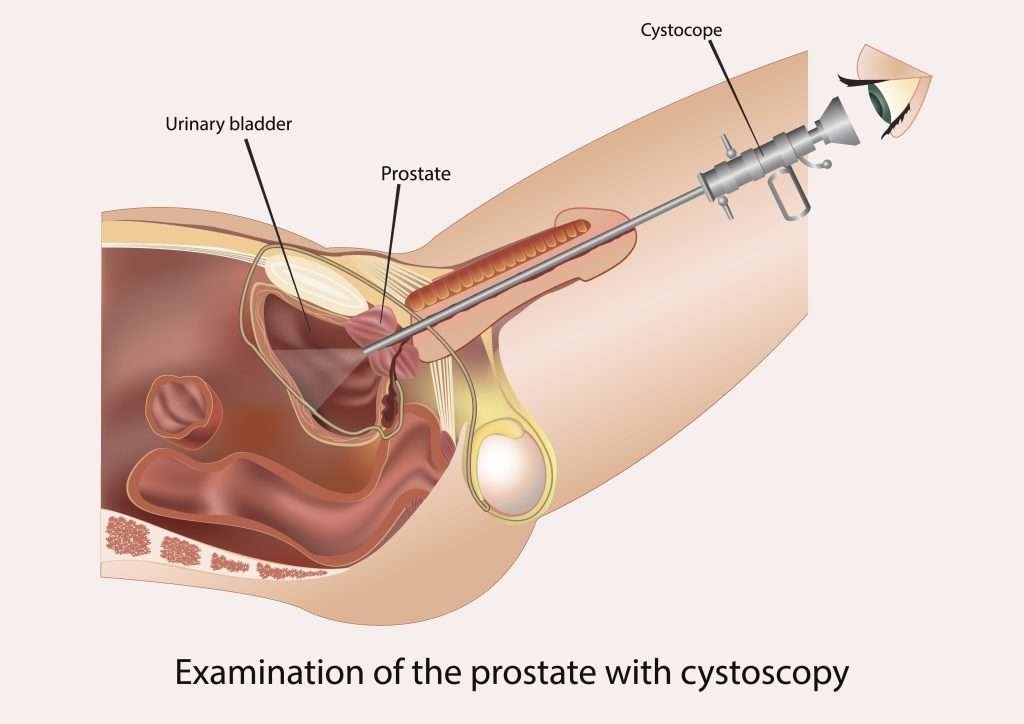
During the procedure, the patient is often asked to lie down while a local anesthetic is applied to numb the urethra. The cystoscope is gently inserted through the urethra and advanced into the bladder. The procedure usually takes about 15 to 30 minutes. Patients may feel some pressure or mild discomfort during the process, but it is generally well-tolerated. Afterward, there may be some mild burning or a frequent urge to urinate, which typically resolves within a day or two. The doctor will analyze the images captured by the cystoscope to make a diagnosis and discuss potential treatment options if necessary.
Can a Cystoscopy Detect Prostate Cancer?
Cystoscopy is not a standard diagnostic tool for prostate cancer, as its primary role is to examine the bladder and urethra rather than the prostate itself. However, it can play an indirect role in suggesting the possibility of prostate-related issues. For example, if the prostate becomes enlarged or abnormal, it may compress the urethra, which could be visible during a cystoscopy. Irregularities in the urethra or bladder neck, such as blockages or narrowing, could point to a prostate condition like benign prostatic hyperplasia (BPH) or, in rare cases, prostate cancer. Nonetheless, these findings are not specific enough to confirm cancer, as they are often associated with other prostate conditions.
The primary limitation of cystoscopy in detecting prostate cancer is that it does not directly examine the prostate tissue or provide detailed images of the prostate itself. Cystoscopy involves visualizing the urethra and bladder but does not assess the deeper prostate structures where tumors may develop. Additionally, cystoscopy does not offer the ability to take tissue samples, which are crucial for diagnosing cancer.
While cystoscopy cannot diagnose prostate cancer on its own, it can complement other diagnostic tools. For instance, when a patient presents with urinary symptoms such as difficulty urinating, blood in the urine, or a weakened urine stream, a cystoscopy may help identify the source of these issues. If the cystoscopy suggests prostate abnormalities, further tests like a prostate-specific antigen (PSA) test, digital rectal exam (DRE), or biopsy may be recommended to confirm whether prostate cancer is present. Thus, cystoscopy can provide valuable information in the broader diagnostic process.
Diagnostic Tools for Prostate Cancer
Several diagnostic tools are used to detect and confirm prostate cancer, often starting with non-invasive methods and progressing to more invasive techniques when necessary.
PSA Test:
The prostate-specific antigen (PSA) test is one of the most common and widely used screening tools for prostate cancer. It involves a simple blood test that measures the level of PSA, a protein produced by the prostate gland. Elevated PSA levels can be a sign of prostate cancer, though high PSA levels can also be caused by benign conditions like benign prostatic hyperplasia (BPH) or prostatitis. A higher PSA level doesn’t necessarily indicate cancer, so the test is typically followed by additional evaluations.
Digital Rectal Exam (DRE):
The DRE is a physical examination where the doctor inserts a gloved finger into the rectum to manually check the size, shape, and texture of the prostate. During the exam, the doctor may feel for lumps, hard areas, or irregularities that could indicate prostate cancer. While it provides useful information, a DRE alone cannot diagnose cancer and is often used in conjunction with other tests.
MRI and Ultrasound:
Imaging techniques such as magnetic resonance imaging (MRI) and transrectal ultrasound provide detailed views of the prostate gland. MRI, in particular, helps in visualizing the prostate’s structure and detecting abnormal growths. Ultrasound is often used to guide prostate biopsies, allowing doctors to obtain precise tissue samples.
Prostate Biopsy:
The biopsy is considered the gold standard for diagnosing prostate cancer. It involves removing small tissue samples from the prostate to be examined under a microscope. If cancer cells are present, the pathologist can determine the type and aggressiveness of the cancer, typically using a Gleason score.
Role of Combined Approaches:
To increase diagnostic accuracy, doctors often use a combination of these tools. For instance, a PSA test may prompt a DRE and imaging studies, followed by a biopsy for confirmation. This multi-faceted approach allows for more reliable diagnosis and tailored treatment options for patients.
By utilizing multiple diagnostic methods, healthcare providers can effectively detect prostate cancer, determine its stage, and create an appropriate treatment plan.
When Might Cystoscopy Be Used in Prostate Cancer Cases?
While cystoscopy is not typically used to detect prostate cancer, it can play a role in certain situations where prostate and urinary issues overlap.
Urinary Symptoms Evaluation:
Cystoscopy may be used to evaluate urinary symptoms that could be related to prostate problems. Conditions like benign prostatic hyperplasia (BPH) or prostate cancer can cause urinary issues, such as difficulty urinating, weak stream, or frequent urination. Cystoscopy can help rule out other bladder conditions, such as urinary tract infections or bladder stones, which may present with similar symptoms. It can also be used to check for bladder obstruction caused by an enlarged prostate or cancerous growth pressing on the urethra.
Monitoring Other Conditions:
In some cases, cystoscopy might be employed to monitor other conditions that could co-occur with prostate cancer. For example, if bladder cancer or other urinary tract issues are suspected, cystoscopy is a valuable tool for assessing the bladder and urethra. Prostate cancer can sometimes be associated with these conditions, especially in more advanced stages. In such cases, cystoscopy helps ensure that no additional bladder pathologies are contributing to the patient’s symptoms.
Advanced Prostate Cancer:
In rare instances, cystoscopy might be used when prostate cancer has advanced to the point where it spreads to the bladder or urethra. This can occur if the cancer metastasizes, or in cases where prostate cancer obstructs the urinary tract, leading to symptoms like blood in the urine, difficulty urinating, or painful urination. A cystoscopy can help identify these changes and guide further treatment decisions.
Though cystoscopy is not a primary tool for diagnosing prostate cancer, it may assist in the management and monitoring of related urinary tract issues in patients with prostate cancer.
Risks and Benefits of Cystoscopy
Cystoscopy is a valuable diagnostic procedure mainly used to examine the bladder and urethra. Although it is not typically used for prostate cancer detection, it can help identify urinary tract issues that may arise alongside prostate conditions. Below are the key benefits and risks associated with cystoscopy:
Benefits:
- Minimally Invasive: Cystoscopy is generally quick, requires only small incisions or no incisions at all, and is less invasive than surgical procedures.
- Urinary Symptoms Evaluation: It can help assess unexplained urinary symptoms, such as frequent urination, blood in urine, or pain, which may be related to prostate issues.
- Diagnosis of Co-existing Conditions: The procedure can help rule out bladder or urethral problems that may co-occur with prostate conditions or prostate cancer.

Risks:
- Discomfort and Pain: While the procedure is typically well-tolerated, patients may experience discomfort or a mild burning sensation during or after the test.
- Infection: Like any procedure that involves the urinary tract, there is a risk of infection, though it is relatively low.
- Bleeding: Some patients may experience minor bleeding following the procedure, especially if the bladder or urethra is irritated.
- Limited Use for Prostate Cancer: Cystoscopy cannot diagnose prostate cancer, as it does not examine the prostate itself or provide tissue samples necessary for a definitive diagnosis.
Overall, while cystoscopy can be useful in evaluating related urinary symptoms, its role in prostate cancer diagnosis is minimal. It’s often used in combination with other diagnostic tools for a more comprehensive evaluation.
Frequently Asked Questions
1. Can cystoscopy replace a PSA test for prostate cancer detection?
No, cystoscopy cannot replace a PSA test. PSA testing is a blood test that measures prostate-specific antigen levels, which can help detect prostate cancer, whereas cystoscopy is primarily used for examining the bladder and urethra, not the prostate.
2. Does cystoscopy show abnormalities in the prostate?
Cystoscopy does not directly visualize the prostate, but it may reveal issues related to the urinary tract that could be associated with prostate problems, such as an enlarged prostate or blockages caused by prostate enlargement.
3. Is cystoscopy painful?
Cystoscopy is generally not painful, but it can cause discomfort or a mild burning sensation, especially during the procedure or after. Most patients tolerate it well with minimal discomfort.
4. What other tests should I consider for prostate cancer diagnosis?
In addition to cystoscopy, other diagnostic tests for prostate cancer include the PSA test, digital rectal exam (DRE), MRI or ultrasound imaging, and prostate biopsy, which is considered the gold standard for confirming a diagnosis of prostate cancer.
5. Are there risks associated with cystoscopy?
While cystoscopy is a minimally invasive procedure, it carries some risks, including discomfort, mild bleeding, and a small risk of infection. These risks are generally low, but it is important to discuss them with your healthcare provider beforehand.
Conclusion
Cystoscopy is not a primary diagnostic tool for prostate cancer, but it can offer valuable insights into urinary symptoms that may be linked to prostate conditions. While it may indirectly indicate prostate abnormalities, it cannot provide a definitive diagnosis of prostate cancer. If you’re experiencing urinary issues or other concerning symptoms, it’s crucial to consult with a healthcare provider for the appropriate diagnostic tests, such as a PSA test, digital rectal exam, or prostate biopsy.
If urinary symptoms persist or remain unexplained, discussing the potential role of cystoscopy with your doctor can help determine if it might be useful in ruling out other urinary tract conditions. Early diagnosis and intervention are key in managing prostate health effectively.